Our solutions
No search results
Care homes
Michał Szymański, MD
Genesis of the disease
Stress urinary incontinence (SUI) is a civilization disease, which, given the nature of the problem, is an embarrassing and very often hidden ailment. The dysfunction associated with the described problem affects the psychophysical condition of patients dealing with this ailment. Stress urinary incontinence, as well as light and heavy incontinence forcing patients to use incontinence products such as urological liners or incontinence pull up’s pants for adults. This type of prevention does not give full comfort, discretion, and most importantly – a sense of security. However, this condition can be treated not only pharmacologically, but also surgically with the use of minimally invasive surgical techniques – through implantation of urological tapes treating this ailment permanently and giving comfort and safety.
The cause of this disease is a not properly functioning urethral closure mechanism resulting from the weakening of the sphincter muscle of the urethra or the hyperactivity of the bladder, urethra, genitourinary fistulas, dilatation of the bladder. The reasons for this dysfunction include, in case of women, inter alia multiple deliveries, damages of the urinary tract, problems with hormonal system, innate defects. For men, the causes of this condition include urethra surgeries.
The scale of the problem in the world
The incidence of urinary incontinence (UI) was estimated on the basis of 35 independent studies on a group of 230 000 people, belonging to different social groups and five ethnic groups. UI incidence in women was 27.6%, a maximum occurred in the 5th decade of life – 33%. Statistical data from departments and gynaecological and urological outpatient clinics shows that this symptom occurs in approximately 25-30% of patients over 45 years of age. It should be noted that a number of patients never report to the doctor. Every year the U.S. spends on the treatment of UI about 17.5 billion dollars (1995). It is estimated that if everyone in the U.S. who suffer from incontinence would look for help, the cost of the treatment and care would amount to $ 41 billion. Urinary incontinence hampers the normal functioning in the society and is the cause of lower self-esteem and overall well-being. The conducted studies on the population of Norwegian women showed that 46% of them identified the discomfort associated with incontinence as tedious, and 34% – as extremely annoying. The problem of urinary incontinence also has its economic aspect. It has been shown that the costs associated with having to buy the necessary medicines and personal care products exceed for about 64% the standard expenses of healthy women. It is estimated that women with stress urinary incontinence in 1998 spent for the direct aids $ 5642 USD, and the indirect measures 4208 $ U.S. These included the purchase of inserts and hygiene products, costs for professional medical help and expenses for surgical treatment. In England the budget allocated for the treatment of urinary incontinence in women is 2% of the total expenses. In the period from 2000 to 2001 there were 8000 surgical procedures because of urinary incontinence for the amount of 10.3 million pounds from the NHS funds. It has been estimated in the United States that the annual direct medical expenses of urinary incontinence are comparable and similar to those that apply to such diseases as breast cancer, osteoporosis and arthritis.
The needs of Polish market
It has been estimated that in Poland there are 20.000-30.000 procedures of urological tape implantation. However, the real need is much higher. It is assumed that approximately 30% of women suffer from this ailment, which makes about 3 million patients in Poland who should have an urological tape implanted. The percentage data concern also the global market. The tapes offered on the Polish market are available only with reusable applicators. Only a few manufacturers offer the tapes with disposable applicators made of artificial materials. The analysis of the costs associated with the purchase of tapes with applicators and comparing them to the prices of the implant can be concluded that it is more economical to purchase a product with reusable applicators. Each hospital has its own sterilisation centre and can sterilise the reusable applicator on its own, thereby reducing the cost of purchasing a disposable one. The number of sold reusable applicators represents about 1% of the amount sold tapes.
Methods of treatment
Surgical treatment is mainly used in the following cases: stress urinary incontinence, mixed form of urinary incontinence. The methods most frequently used in the surgical treatment of urinary incontinence are:
- suspension of the urethra using the tension free tape through the vagina (e.g. Tension-free Vaginal Tape (TVT), Trans Obturator Tape (TOT));
- extraperitoneal vaginal suspension (Burch colposuspension method, operations by Marshall-Marchetti-Krantz method);
- needle procedures;
- urethral injections (usually with Teflon or collagen);
- loop operations (almost entirely supplanted by TVT and TOT);
- implantation of an artificial sphincter (the highest degree of difficulty, a very rarely used treatment).
Selecting the optimal treatment method is often very difficult and depends on many factors, including: the patient’s body weight, the patient’s age, number of births and the complications associated with them, poor general health, the desire to have children, coexisting chronic diseases, doing competitive sports, experience of the operator.
The effectiveness of the chosen treatment method also depends heavily on the well performed diagnostics, which allows to determine the cause of urinary incontinence and the presence of any accompanying genital pathology.
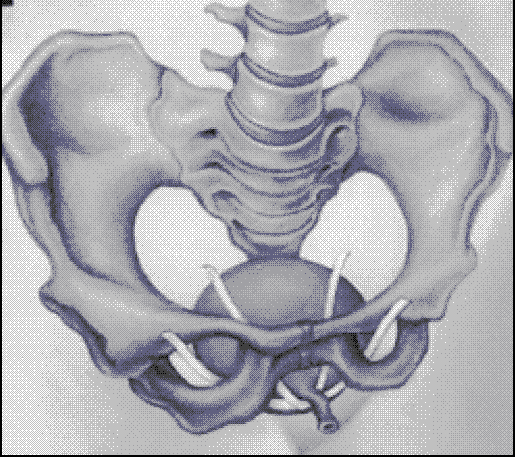
Characteristics of TOT and TVT implantation methods
In the two treatments (TOT and TVT) the implanted product is a tape made of synthetic polymers (such as polypropylene), or of allogeneic material. Leading manufacturers of synthetic tapes are Ethicon, AMS. These tapes can also be partially resorbable e.g. the T-Sling by Polhernia company.
The set for stress urinary incontinence consisting of a urological tape and a system of applicators for TVT and TOT methods is the subject of the description of implantation methods.
In the surgical treatment of urinary incontinence in women the TVT method (Tension-free Vaginal Tape) and the TOT (Trans Obturator Tape) method is most often used – the Dallop® NM tape is intended for both of them.
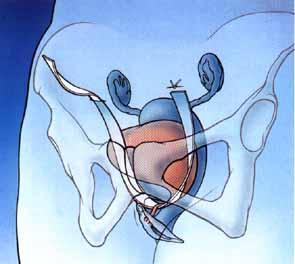
TVT method
This TVT method of surgical treatment of stress urinary incontinence in women enjoys great popularity among surgeons. This procedure is performed under local anaesthesia. It takes about 20 minutes. During this procedure, the tape is introduced through the retro-pubic space, and the ends are drawn up on the abdominal fascia. This is done using special applicators designed for the specificity of the procedure. The applicators allow you to place the tape under the urethra in a safe way, providing high efficiency of the procedure, estimated at about 85% in the long-term evaluation.
The TVT method is a procedure used in the treatment of stress urinary incontinence in women performed with vaginal access, aimed at suspending the middle and posterior part of the urethra.
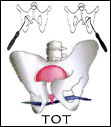
TOT method
The second method used more and more commonly in the surgical treatment of urinary incontinence in women is the TOT method. It is a modification of the TVT method limiting the risk associated with it. It primarily reduces the risk of puncturing the bladder or damaging the pelvic or major blood vessels. This treatment is also performed under local anaesthesia, and the duration is shorter. The big difference is the way through which the tape is implanted. For the TOT method special applicators were designed to enable taking the tape through a small space in the foramen obturatum, which reduces the risk of penetrating the bladder and allows the location of the band in a more precise and safe. This provides a method for increasing the efficiency of approximately 95%.
The method TOT uses the access through the foramen obturatum, through which the urological tape is pushed. It aims to create a kind of hammock supporting the urethra in the middle and back part.
Optimal materials /raw materials for urological tapes
Many authors of publications describing the use of various types of urological tapes, assessing the effectiveness of implanting tapes made of material of both human and animal, and synthetic origin said that the use of the tapes made of materials of human and zoonotic origin carries a high risk of complications. The most common are: erosion, infections, absorption of the tape and reduction of the initial parameters of the tapes. In addition, it is difficult to assess the effectiveness of the treatments with their use. However, the use of polypropylene tapes is free from most of these complications. Besides, the polypropylene tapes are characterised by a relatively small loss in the value of the initial parameters, what considerably affects the efficiency of procedures performed.
A randomised study on two groups of New Zealand rabbits to evaluate the response of the bladder tissue in contact with synthetic implants (the TVT tape) and zoonotic implants (SIS – Small Intestinal Submucosal – transplant of porcine origin). The third group was a control group which was subjected to a similar procedure as the other groups, with the difference that it did not have any implant. Observations were carried out for two periods of implantation – 6 and 12 weeks. As a result of these studies it was found that the wall of the bladder in contact with polypropylene showed no inflammatory reaction. Only in 3 of 12 animals the presence of fibrosis was observed. In the test group treated with porcine SIS implant in one animal a strong inflammatory response was observed, in two animals fibrosis was found. In the control group, as expected, there were no changes in the tissues of the bladder. On the basis of these observations, the authors evaluated the conclusion that both materials – both the polypropylene and the porcine SIS implant appears to be safe in contact with the tissues of the bladder. In addition, the polypropylene implant retained its morphological characteristics in the two periods of observation.
Many doctors evaluated the mechanical properties of TVT polypropylene tapes and tapes of human origin (CFL) after their implantation. These studies were carried out on rats, by selecting two observation periods 6 and 12 weeks, because in patients undergoing surgery with the use of tapes the acute tissue reaction to the presence of foreign materials usually occurs in the first three months. Two parameters of the tapes were tested: average breaking load and maximum load at break. The authors assessed that the TVT tapes retain their morphological and strength characteristics after the assessed implantation periods. However, the tapes of human origin (CFL) definitely lose their strength. Both the evaluated parameters, both after 6 and 12 weeks of observation, for the TVT tapes were almost three times higher than for the tapes of human origin (CFL). The doctors in their summary stated that such a significant decrease in the strength parameters can be the cause of low efficiency of the procedures with the application of the tissues of human origin (CFL).
Characteristics of Dallop® NM tape
Urological tape Dallop® NM meets the essential requirements of Directive 93/42/EEC for products classified as Class IIb medical devices. According to the above-mentioned Directive, Annex 9, Rule 8 “All implantable devices and invasive surgical devices for long-term use are in the Class IIb.”
Dallop® NM urological tapes are made of:
- monofilament polypropylene yarn with a thickness of 0.16 mm (185 dtex) – used to produce the main part of the tape;
- polypropylene yarn with a thickness of 0.3 mm (640 dtex) – used to make the handles allowing to fix the tape on an applicator.
Both materials are made of 100% polypropylene homopolymer and are coated with preparations in an amount of not more than 0.25%. Both yarns have a minimised elongation factor (up to 0.5% in water at 40°C ± 2°C) and the corresponding tensile strength. Drains protecting the areas where the tape and the handles are connected are made of medical PVC granulate and are used to protect the tape and the tape handles against pulling out when the tape is put through anatomical structures.
Parameters of Dallop® NM tapes:
|
No. |
Parameter |
Requirements |
|
| 1. | Breaking strength | min. 16 N | 117 N |
| 2. | Pore size | min. 75 µm | 0.38 mm2 |
| 3 | Width | 1.0 – 1.2 cm | 1.1 cm |
The Dallop® NM tapes have smooth edges and do not require additional protection, because the implant does not cause the risk of tissue damage.
The Dallop® NM tape is packaged in double medical packaging – BOM paper-film reel with a gusset suitable for ethylene oxide (EO) sterilisation. A medical device after packaging undergoes sterilisation with ethylene oxide (EO) in accordance with the requirements of EN ISO 11135-1.
The Dallop® NM tape is available in 2 sizes with a length of 60cm and 45cm, the handles are blue and made of polypropylene yarn, and the covers (drains) are made of heat-shrinkable material.
Application of the tape
The Dallop® NM tape is designed for use in the surgical treatment of female urinary incontinence by means of TVT and TOT methods. These methods are used to treat stress or a mixed form of urinary incontinence. The tape is intended to replace weakened pelvic floor muscles, which are not able to provide an appropriate angle of the urethra, leading to urinary incontinence. Creating a support under the urethra the tape restores it to its natural position.
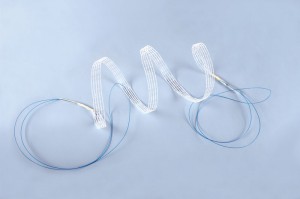
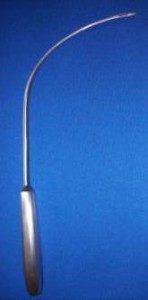
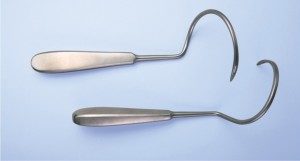
Applicators
The provide safe implantation of the Dallop® NM tape appropriate applicators were designed: a modified TVT needle, a modified Emmet needle and curved Emmet needles (left and right). Modifications to all the applicators included adapting their ends to the fixing handles of the tapes so that you can attach the tape holder on the applicator to securely introduce the tape.
The raw material used to manufacture the applicators is stainless steel of composition appropriate for the production of medical instruments. The applicators are packed in double polythene film and a cardboard box.
The Dallop® NM tape is sold separately or in a set with applicators for a TVT and / or TOT method.
Clinical studies
Research on the Dallop® NM urological tape – produced by Tricomed S.A. and placed on the market after obtaining the CE mark and the certificate of registration was carried out in Matopat Specialist Hospital in Toruń during 01.09.2010 – 01.09.2011. Three medical obstetrics and gynaecology specialists took part in the study: Janusz Stankiewicz MD, PhD., Michał Szymanski MD, PhD, Piotr Wojtynek MD, PhD. Each of the physicians choosing patients for the clinical trial was both the operator and the person collecting clinical data from the intra- and postoperative period. The aim of this study was to evaluate the efficacy and safety of the Dallop® NM urological tape in the surgical treatment of stress urinary incontinence in women. The study included an risk assessment of complications after the implantation of the tapes and their subsequent impact on the quality of life of the patients.
Materials and methods
20 patients (women) with diagnosed with stress urinary incontinence or a mixed type of this disorder with a predominantly stress component took part in the assessment. Each patient had one Dallop® NM tape implanted; the surgical procedures were performed in the period 13.09.2010 – 08.03.2011. Characteristics of the study group: 4 patients before surgery additionally had urinary urgency. Patients’ age 35 – 74 years, (average age 52 years), BMI between 19 – 41 (average 27). All patients in the preoperative period and during the qualification for the surgery had their medical history collected, and an gynaecological examination with ultrasound performed. In all the patients the test result was positive. Before the surgery urine cultures were performed in order to exclude an urinary tract infection, the urodynamic test confirmed the presence of stress urinary incontinence.
The results took into account the data collected during the operation, after 30 minutes from the surgery, at discharge from the hospital, and within a period of one, three and six months after the surgery. All tapes were implanted with access through the foramen obturatum (TOT), this access is now preferred in most centres dealing with the surgical treatment of stress urinary incontinence as giving fewer complications, shortening the treatment time and eliminating the need for intraoperative cystoscopy compared with the vaginal access (TVT).
Description of the surgical technique: After preparing the operating field a longitudinal incision in the vagina was performed, the vaginal wall was dissected of the urethral, tunnels were created to the sides towards the obturator foramens. Through incisions in the groin folds on both sides an Emmet needle was introduced directing it through the obturator foramens to the previously prepared tunnels. The handles of the Dallop® NM tape connected to the ends of the tape were rove through the hole in the needle and the ends of the tape were led “from the inside out” by withdrawing the needle. The tape was laid without tension under the urethra, then the vaginal wall was sewed. A vaginal compression tampon was applied for a day, after the surgery the catheter was removed from the bladder, the patients urinated on their own. Eighteen operations were carried out under general anaesthesia, in two cases under regional anaesthesia – the type of anaesthesia was chosen by the anaesthesiologist in consultation with his patient.
Results of the studies
The total time of the operation: the 18 TOT operations took 10 – 30 minutes (average 19 minutes). Two operations connected with additional operating procedures (removal of the uterus, vagina wall carvings) lasted 60 minutes; the average for all the 20 patients: 23 min. Assessment of the convenience of using a tape during a surgery (0-5), (0 – cumbersome and difficult to use, 1 – very complicated application, 2 – complicated application, 3 – high degree of difficulty, 4 – small degree of difficulty, 5 – handy and easy application). In two cases the operators rated the tape at 4, in the other cases – 5 (average 4.9). After 30 minutes of surgery the pain strength according to VAS was in the range of 2 – 4, on average 2.3. The type and duration of used painkillers: all the patients were given Ketonal intravenously at a dose of 1 amp. every 8 hours, 9 patients additionally were given Morphine 1 amp. every 6 hours, 5 were given Tramal intravenously 1 amp. Noticeable discomfort on a scale 0-5 (0 – pain, I want to remove the tape, 1 – huge discomfort, 2 – big discomfort, 3 – moderate discomfort, 4 – slight discomfort; 5 – no discomfort) ranged from 4 – 5, average of 4.4. Postoperative complications such as hematoma, urinary retention, need to remove the tape, the temperature above 37.5°C, there were no signs of infection in any of the patients. Hospitalisation time took 1 – 3 days (average 1.95). At discharge from the hospital, the cough stress test result for all the patients was negative, the patients did not report any episodes of urinary incontinence. The pain strength according to VAS was 0 to 2, on average 0.6. Noticeable discomfort in the scale of 0-5 – three patients reported mild discomfort, others no discomfort (4.85 average). Postoperative complications were not observed in any of the cases. One of the patients at discharge reported occurrence of urinary urgency “de novo”. All patients reported to a control check after a month from the surgery. None of them reported any incidents of stress urinary incontinence.
Two patients with the mixed form of urinary incontinence reported the continuing urinary urgency of a similar intensity as in the preoperative period, the treatment with anticholinergics was continued. Pelvic examination: in all patients the post-operative wound healing process was correct, there was no erosion, no hematoma, no need to remove the tape, etc.. Test cough test was negative – 100% of the respondents. The pain strength according to VAS: one patient assessed as “1”, the others as “0”. Noticeable discomfort (scale 0-5) – one of the patients evaluated at “2”, one at “4”, the others at “5”, the average 4.8. 3 months after the surgery in any patient in the entire study group there was no incontinence observed. The female patient who experienced postoperative urinary urgency, treated conservatively because of the lack of improvement, severity of the symptoms, was directed to urology (cystoscopy) consultation. The cystoscopy revealed diffuse leukoplakia of the bladder, the sites of leukoplakia were dissected and coagulated (this condition was not associated with the implantation of the tape). After the cystoscopy subjective improvement and a reduction in the urinary urgency was observed. The other two patients treated with anticholinergics: in one the urinary urgency was eliminated, in the second one it was significantly decreased compared with the preoperative period. Pelvic examination: in all patients the state was correct. Cough test negative – 100% of the respondents. The pain strength according to VAS: “0”, all the patients. Noticeable discomfort: two patients “4” – slight discomfort, while the others “5” – no discomfort, the average of 4.9.
After 6 months all the patients reported for the check-ups. there was no health deterioration, there were no symptoms that may have been associated with the surgery, there was no stress incontinence. None of the patients agreed to the proposed urodynamic study before the follow-up visit considering that the treatment process is complete. Pelvic examination: in all the patients the state was correct, cough test negative. Pain strength according to VAS: the patients estimated at “0”, noticeable discomfort at “5” – 10%. The time to return to full active life after the operation ranged from 1 – 8 weeks, on average 2.9 weeks. The patients assessed that their condition improved after surgery.
Summary of the studies
In the study group of 20 patients with stress or mixed type of urinary incontinence during the 6 months from the implantation of the Dallop® NM urological tape by means of the TOT method, there were no significant intra – and postoperative complications associated with the implant. The tape was evaluated by three operators involved in the study as a handy, convenient to use and safe. The duration of the implantationof the Dallop® NM tape with access through the foramen obturatum access was short (on average about 20 min.). The pain and discomfort associated with the surgery in the patients was short, low-graded. Most of the patients returned to active life after the operation within 2 – 3 weeks, within six months all patients found their health as better compared with the preoperative period. Efficacy in the treatment of stress urinary incontinence in the study group was defined as 100% in terms of subjective (interviews collected from the patients) and objective (pelvic examination with a cough test) opinions.
Conclusions
- Based on the results of the six-month observation of the operated group of twenty women, the Dallop® NM urological tape can be considered as an effective, convenient for doctors and patients, and safe method for the treatment of stress urinary incontinence in women.
- In the examined group all the patients achieved good results of the surgical treatment and there were no complications associated with the surgical procedures and the implanted tape.
Elżbieta Szwałkiewicz
National Consultant in Nursing Chronically Ill and Disabled People
One of the indicators used to assess the quality of long-term care of an immobilised person is the skin condition in areas exposed to constant pressure. It would seem that nurses know everything on the prevention of pressure ulcers, and that is why I wonder what is the reason for such a high incidence of pressure ulcers in people who are under constant nursing supervision.
The scale of the problem entitles me to claim that in our country we have common and very serious failings in the care of the sick and disabled, both in stationary health-care and social assistance, as well as in home conditions. These neglects are the cause of immense suffering and generate substantial costs of treatment and care.
There have been many publications on the subject of pressure ulcers referring to numerous medical research and statistics. They repeat the same key information:
- the major etiological factor is the pressure on tissue located over bone prominences, leading to the development of necrosis and then to ulceration,
- skin damage occurs as a result of repeated pressure exceeds the average pressure in skin capillaries (32 mmHg), the impairment of sensation is a contributing factor,
- the formation of pressure ulcers is accelerated by skin maceration, which is a consequence of increased humidity due to urine and faecal incontinence or perspiration,
- the most common location is around the sacrum, ischiadic tubers, trochaners, ankles and heels,
- each immobilised patient is at risk of pressure ulcer formation,
- modern technologies ought to be used to reduce the pressure on the skin, such as specially designed mattresses, pillows, textiles and equipment for sliding movement, modern protective and therapeutic dressings, and aids absorbing urine,
- the treatment cannot be focused on the topical management of decubitus ulcer.
Basic principles relating to prevention:
- proper nutrition – adequate intake of protein, calories and fluids will prevent the occurrence of negative nitrogen balance, weakness and dehydration,
- reduction or elimination of pressure and friction on the skin – this effect is achieved through the use of pressure relief mattresses and pillows, frequent change of body position, application of proper rules for lifting and moving patients,
- strictly comply with the basic care principles of people with incontinence (also the faecal type), including:
- daily washing and cleaning after every contamination with excretions,
- systematic control of skin condition in areas exposed to moisture,
- using absorbent products adequate to the level of micturition,
- preventing skin inflammation through the use of special protective dressings,
- protecting the skin against overdrying and irritants (urine and sweat) through the use of appropriate skin care products.
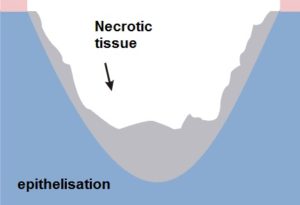
Modern approach to the treatment of pressure ulcers and other chronic wounds favours wound healing in a humid environment with the use of various specialist dressings, which are applied depending on the type and the location of the wound.
Scientific studies and practical experience have shown that increased moisture in the wound stimulates epidermisation, and this, in turn, stimulates the growth of connective tissue underlying the skin. Specialist dressings compared to conventional gauze dressings also affect the rate of healing. They prevent the damage to the young epidermis during each dressing change, and they contain substances that affect the treatment and healing of wounds. Not to be underestimated is the fact that effective protection of the interior of the wound against external factors, and to perform normal hygiene procedures without changing the dressing.
Therapeutic proceedings (including the selection of a dressing) and the cost depends on the type of wound and the stage of healing . Some wounds are treated for many months, sometimes over a year. There are often problems in the healing process, and the most dangerous of them cause infections. An unsecured wound may be infected with bacteria, viruses or fungi. They proliferate spontaneously and poison tissues with their secretions. The wound infection can spread quickly up to the form of sepsis, which threatens the patient’s life. The cost of treating infected chronic wounds significantly increases mainly due to the need to use more specialist dressings and the use of expensive antibiotics.
As a national consultant I observe with great concern that the number of people who suffer from pressure ulcers and other chronic wounds is not decreasing despite years of educational campaigns. The responsibility for this situation falls not only on the nurses but also on those responsible for creating the conditions for the care of sick and dependent people, and the National Health Fund as a payer financing the costs of treatment. It is difficult to understand the fact that the National Health Fund does not require health care centres to report on patients with bedsores and the course of treatment. Isolating procedures concerning the treatment of bedsores, and leaving the treatment costs within the institution in which they occur, would highly affect and activate the creation of suitable conditions for the prevention of pressure ulcers. It should of course take into account the fact that some chronic wounds are not the result of negligence but result from the patient’s physical condition; most often it relates to end-phase of long-term biologically devastating neoplastic disease.
As part of my own professional practice I was able to watch quite remarkable effectiveness of modern specialised dressings in the treating of pressure ulcers. Of course, the nurses should be aware of all the known methods of chronic wounds treatment, not only of pressure ulcers but also ulcers, malignant ulcers, diabetic foot ulcers and burns. The bottom line is to be aware that it is unacceptable not to obey the basic prevention principles and to expose the patient to the formation of pressure ulcers or other chronic wounds. Both health and financial consequences of economising on absorbent products and protective dressings are very serious, not only for the patient but also for the nurses and the unit they work for.
Elżbieta Szwałkiewicz
National Consultant in Nursing Chronically Ill and Disabled People
Even the most modern, well-matched to the wound type dressing will not facilitate the wound healing process if additional conditions conductive to further body regeneration will not be met.
These are:
- proper body hygiene,
- skin protect against irritating effects of urine,
- suitable bed, mattress, bed linen and underwear,
- elimination of pressure on the part of the body affected by a bedsore,
- safe movement and positioning of the body,
- adequate nutrition and hydration.
Modern technical solutions and technologies allow for the safe performance of hygienic activities, even in those patients with very sensitive skin and completely immobilised, without the risk and effort associated with their movement. On the market there is a wide range of skin care, hygiene facilitating devices available. When dealing with dry skin (frequently washed with soap), weakened, macerated, constantly subjected to the action of irritants, it is necessary to check the condition of the skin daily looking for signs of an allergic reaction. Appropriate preparations for cleansing and skin care of the sick are the ones that can be applied to sensitive and irritated skin, and have moisturising, greasing and elasticising properties. They should alleviate symptoms of inflammation, grease and protect the skin against irritants such as urine. For irritated and itchy skin soap should not be used only mild cleaning agents (lotions, foams). It is advisable to use cosmetics with as little allergic reactions as possible. The used cleaning and care products should be manufactured in sets by the same company as this will prevent the use of products of different chemical components coming into harmful interactions for the organism. Just wash the wound area, and always check the condition of the wound dressing and protection of the wound against pollution and getting wet during hygiene procedures.
Unpleasant for the patient and his/her environment urine odour can be eliminated by proper selection of absorbent materials and their appropriately frequent change – about four times a day. While changing be sure to cleanse the abdomen, genitalia, groin and buttocks.
A patient who cannot change the position from lying to sitting can be washed traditionally in bed, but can be also bathed in a special movable bathtub. The bathtub is taken into the patient’s room, one side wall is removed and is set along the bed. Then, using a cloth or a special sliding mat to move the patient (previously undressed and covered) into the tub. If the patient is on a drip, monitor, respirator, etc., the bath is carried out in the room next to the bed. This is possible when to the sink tap (located in the room) a shower hose of suitable length with a shower head is attached. Similarly, the drain hose must be of appropriate length to reach to a special outlet installed under the sink. If the patient is able to leave the room, he/she is taken on the bathtub to the bathroom with a shower post. The drain hose is introduced into the floor drain. Bathing in the supine position can also be done in a bathtub with an adjustable height. A person who cannot move, is moved (undressed and covered) by sliding onto a special man lift – a kind of trolley-stretcher. Following the transfer of the patient to the bathroom, the lift is placed on the bath, which rises (electric mechanism operated by means of a remote control) to the height appropriate for the carer, so that he/she does not to have to bend down. Then, the lift with the patient is lowered to the bottom of the tub. Most of the mentioned bathtubs has also an incorporated hydro massage device. The lift has the ability to raise the head rest so that the patient can be washed in a sitting or reclining position. In a set with the bathtub there are also available chair lifts that help people with paraplegia or the disabled to get to the bathtub and leave it. These people can also wash themselves in the shower using the lift or a sanitary chair. All institutions where there are patients with locomotor disabilities should have integrated systems for personal hygiene i.e. movable equipment integrated with cleaning equipment.
People unable to walk e.g. with paraplegia can use the toilet alone but there must be conditions created enabling the move from the wheelchair onto the toilet. The height of the toilet and the wheelchair should be similar. The side walls of the chair and security handles at the toilet should be tippable. Within easy reach of a person using the toilet there should be a shower head to wash and toilet paper to dry the skin. The ability to wash oneself with running water is highly important, because it is very difficult to clean the genital and anal area with toilet paper. In elderly people the skin is wrinkled and therefore its thorough cleaning off stool remnants is not possible by means of dry toilet paper, and repeatedly rubbing the sensitive and dry skin often leads to its damage. In the toilet there should be enough space for a disabled person to drive a wheelchair, park along the toilet, and after picking up the side part of the chair and the toilet handle, move onto the toilet. All people, regardless of their health and fitness, should be able to use the toilet. It should be kept in mind that when lifting and moving the patient strong point pressure on the body ought to be avoided and the sliding method to rotate the body ought to be applied. The need to clean and protect the skin is particularly important for people with disabilities who face the problem of urinary incontinence.
Please note that urine in contact with the skin is an external irritant, causing inflammation. The inflamed skin is red, irritated and painful. There appears also often swelling, itching and flaking of the skin. Patients trying to reduce the annoying itch scratch themselves, and ultimately break the continuity of the skin, leading to the formation of wounds. These scratches are the site of bacterial infection and the development of complex infected bedsores.
The desired effect can be achieved using hygienic disposable absorbent materials, sets for urine collection, specialist personal hygiene and cosmetic and protective preparations. Their offers is very rich in the market.
Diapers, anatomically shaped diapers or urine pads should be chosen according to their absorbent ability, the content of a urine binder, the type of protection against the leakage from the diaper, the ability to reduce unpleasant odours and the possibility to closely adjust to the body. It is also important that the absorbent body is covered with special nonwoven, which also separates the urine absorbed from the skin.
Urinary incontinence leads to constant moisture and maceration of the skin, which promotes its inflammation, damaging, resulting in the formation of bedsores. Therefore, it is necessary to systematically check the condition of the skin in areas exposed to moisture and the state of dressings, and maximally shorten the time of skin contact with urine.
Therefore, the selection of an absorbent product should be determined by the degree of urinary incontinence, the patient’s level of consciousness, time of the day and level of activity. People with pressure ulcers or very sensitive dry skin prone to irritation, should use the so-called breathable diapers. They differ from other diapers for instead of the protective film they have to a special air-permeable laminate.
While nurturing a bedridden person with urinary incontinence (UI) it necessary to use hygienic underpads to maintain the cleanliness of linen or to secure the chair. Do not use rubber underpads but pads made of cellulose with one side coated with special film protecting the chair or the bed against wetness. Here also breathable absorbent products should be applied. People with bedsores should avoid overheating in warm clothes and airless or overly heated rooms, and above all, they should avoid long-term pressure on the damaged skin and skin friction over the ground. This effect can be achieved by using a special sliding and equipment for sliding repositioning, pressure relief mattresses and pillows, frequent change of body position, the application of proper rules for lifting and moving the patient.
Significant reduction or elimination of pressure on the skin can be achieved by equipping the bed with an anti-bedsore mattress:
- alternating pressure (so-called dynamic) anti-bedsore mattress where a motor pumps air into individual chambers of the mattress, filling them only some of them which allows to temporarily relieve another part of the body. Using the mattress does not cancel the obligation to adequately frequent change body position.
- constant pressure anti-bedsore mattress, pumped using a hand pump, enabling to achieve appropriate pressure and reduce the pressure on the body surface. It is also important that it is made of a material with a unique antibacterial formula inhibiting the growth of bacteria and odour inhibitor. Using this mattress has a preventive effect and accelerates healing of existing wounds. This mattress is particularly useful in patients who dislike the sound of the pump motor in the dynamic mattress.
The time of healing a bedsore or any other chronic wound depends on the general state of health and on good nutrition with adequate supply of protein, calories and fluids.
Causes
The diabetic foot syndrome deals with changes appearing on the lower extremities in patients with diabetes.
The cause of the diabetic foot syndrome are changes in the blood vessels (ischemia), and damage to the nerves (neuropathy). Deterioration of vascularisation and innervation in diabetic patients usually progress simultaneously, but only one of these changes is dominant. The dominant factor determines the type of the diabetic foot syndrome, and so can be distinguished: ischemic diabetic foot syndrome or neuropathic diabetic foot syndrome.
Figure: diabetic foot syndrome – classification as for the dominant factor
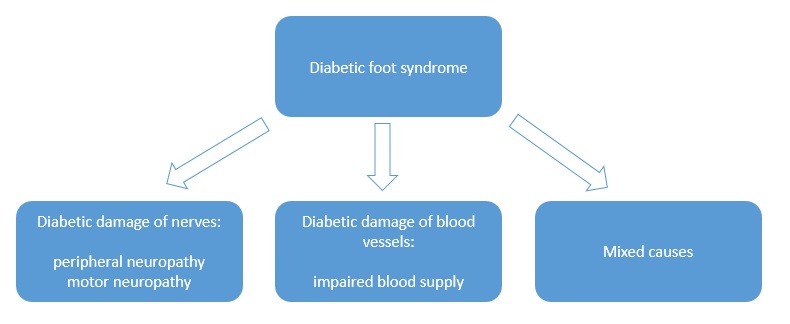
Peripheral neuropathy i.e. peripheral neuritis – is one of the complications of prolonged hyperglycemia and affects both somatic and autonomic nerve cell projections in both legs. The patient has reduced sensation of pain, temperature and touch in the affected leg, and since feels no pain after an injury or compression, the skin is often damaged and ulcers are formed, which are often not noticed early enough and thus start to be treated too late. Late detection of the ulcers may be then too advanced to be successfully treated.
Motor neuropathy causes loss of muscle and foot tendons and, consequently, destruction of the joints. This in turn leads to the concentration of workload on a few small areas of the plantar surface, and further to the formation of callus. The final step of these changes is foot deformation.
Angiopathy i.e. damage to blood vessels – blood supply disorders are characterised by abnormal blood flow in the legs especially tibial and fibular artery. Uncontrolled diabetes favours the development of arterial diseases. The control of blood glucose content is one of the prevention ways, it is also a precondition for starting the process of wound healing.
Therefore, we can distinguish:
- neuropathic foot ulcers, which constitute two thirds of all diabetic foot ulcers
- angiopathic foot ulcers (~ 10%)
- mixed foot ulcers (~ 25%)
Risk groups
- People with diabetes mellitus.
- People with undiagnosed diabetes!
This disease affects mostly people with type II diabetes i.e. the one not requiring insulin injections.
The complication in for of diabetic foot is present in approximately 20% of hospitalised patients because of diabetes, and is the cause of 50% of all limb amputations performed in surgical wards.
Symptoms
Neuropathic diabetic foot
The predominant symptoms:
- loss of sensation to touch, pain and temperature
The patient does not feel the presence of a malicious stimulus such as a cut, burn, hurting by wearing tight shoes, the presence of a foreign body in the shoe. Insensitivity to pain is the basic element causing the formation of ulcers on the foot sole. The neuropathic diabetic foot is warm, with preserved flow in the arteries, but the foot joints and bones are deformed.
In some patients the changes appear in the joints and are formed by gradual destruction of small joints of the foot which results in considerable distortion of the feet. It is necessary then to wear special shoes made upon an individual order. Wearing normal ill-fitting shoes very often leads to the formation of ulcers.
Ischemic diabetic foot syndrome – angiopathic
The predominant symptoms:
- increased sensitivity to pain
The main symptoms are: pain intensifying usually at night, often accompanying painful muscle cramps, tingling or numbness in the leg.
Depending on the level of stenosis and occlusion of arteries in the lower limb, necrosis appears on different areas of the foot.
The most severe form of the disease is the closure of large arteries in the lower limb above the knee. This results in tissue necrosis in the foot, and sometimes also in the lower leg. Necrosis affects mostly toes. Ischemic diabetic foot is characterised by preserved innervation while simultaneous impaired blood supply in the limb.
An untreated diabetic foot syndrome leads to the amputation of the limb.
Location
In patients with diabetic neuropathy ulcers are located primarily in areas of repeated injuries and affect usually the plantar surface of the foot around the metatarsal bone, heel and toes. Usually the neuropathic ulcers are painless.
In addition, as a result of neuroarthropathic disturbances, the foot is distorted in a characteristic way – grooved feet, mallet toes, changed way of walking, and in over-loaded points in the calluses (corns) are formed that can later cause non-healing wounds and ulcers.
In the case of ischemic diabetic foot chronic hypoxia causes that the foot begins to die – it swells, ulcers, necrosis and cracks appear, nails get deformed and soft tissues disappear and the whole foot becomes blue.
Treatment
A specialist in the field of diabetes, surgery (including vascular surgery) and orthopaedics is the competent person for ordering treatment. Nurses also actively participate in the therapy. The most important thing is to keep sugar level in blood in optimal physiological limits.
The treatment is both causal and local.
Wounds are surgically debrided, narrowed blood vessels are unblocked, various vascular grafts are used to allow bypass clogged arteries which improves blood flow in the foot. Along with the surgery blood sugar in the body is controlled and medicaments facilitating the treatment are dosed. In addition to insulin and antibiotics the patient receives medicines that improve blood circulation in the limbs, reduce blood viscosity, enabling to reach the ischemic structures, improve wound healing and scarring. Also appropriate diet is recommended.
Prevention
It most essential in the prevention of diabetic foot development is the proper treatment of diabetes, the control and maintenance of a normal blood sugar level.
After diagnosing diabetes the patient should:
- quit smoking
- gently and carefully take care of the feet
- systematically control the circulation and innervation of the feet
If there are foot lesions, early physician intervention often prevents the need of amputation of the lower limb.
Everyday foot care in people with diabetes should consist of:
- everyday observation – controlling blood flow and sensation, washing in warm (not hot) water, gentle and careful drying – especially the space between toes
- care for nails – regular trimming (but not too short)
- careful selection of shoes – should be sufficiently wide, the right size (patients with neuropathy, due to the worsening of sensation tend to buy too small shoes, smaller than the ones worn so far), the heel should be low and wide, shoes with laces are recommended
- before putting on shoes the patient should check whether inside there are no sharp objects, outstanding seams or rolled inserts
- wear non-binding and non-elasticated socks made of natural fibres (too tight socks can impede blood circulation)
- protect the foot against excessive: soaking , exercises or heating (for example by means of an electric blanket or other energy sources)
- do not use ointments on foot corns – unless your doctor tells otherwise
Any observed changes in the foot, such as swelling, colour change, loss of sensation should be consulted as soon as possible with a doctor.
Even minor cuts, skin cracks and wounds cannot be ignored and always need to be secured with sterile dressings and shown to the doctor during control visits. If there is no progress in the healing it is recommended to urgently consult the doctor.
>
Causes
The causes of leg ulcers are diverse, internally complex and almost exclusively of endogenous-internal origin.
Without a doubt, however, the most common cause of leg ulcers is venous hypertension and arterial insufficiency.
Other possible causes of leg ulcers:
- hypertension: necrotising vascular dermatitis – necrotic angiodermatitis (Martorell syndrome)
- infections: osteomyelitis, tuberculosis, pyoderma gangrenosum, leprosy, insect bites
- vasculitis: polyarteritis nodosa, rheumatoid arthritis
- haematological disorders: haemolytic anemia, fibrinolytic disorders
- neurological disorders: poliomyelitis, peripheral neuropathy (diabetes)
- cancer: mixed basisquamous carcinoma (Marjolin’s ulcer), melanoma, Kaposi’s sarcoma, lymphoma
Ooccurrence
- 75% of all vascular ulcers are the result of venous hypertension – venous ulcers
- 15% is generated as a result of atherosclerosis – mixed ulcers
- 10% is arterial ulcers
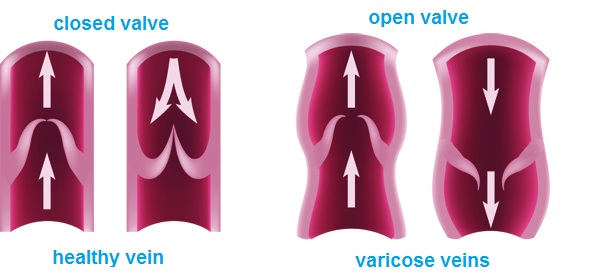
Venous ulcers are caused by severely impaired activity of leg veins. In advanced venous insufficiency of the lower limbs, venous circulation in the lower limbs is disturbed and venous valves are damaged – which results in congestion and increased pressure in the veins. Valves control the blood flow so that it flows only in the direction towards the heart, not to move back. In case of damage or malfunction of valves blood flows back to the lower limb. Blood pressure in the venous system increases, which, if untreated, causes further damage to the valves and superficial veins. Walls of veins lose their flexibility and elasticity, get thicker. For the purpose of treatment and prevention of recurrence of ulcers, it is very important to identify the locations of venous insufficiency.
Risk group
- obesity
- work in a seated or standing position, leading to the stagnation of blood in leg
- hereditary factors – presence of varicose veins in parents
- age, mostly at risk are people over 60 years of age
- sex, statistically varicose veins are more common in women than in men
- number of pregnancies (the more births the greater the risk of varicose veins)
- constipation
- flat feet
- oral contraception
- tallness
Symptoms
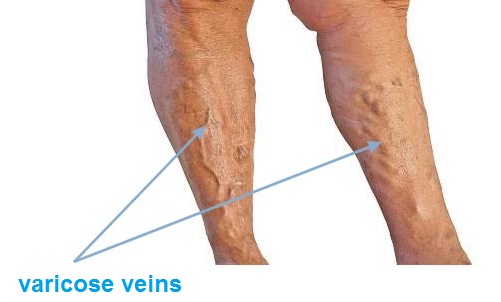
The initial phase of venous insufficiency: feeling of heavy legs, especially in the evening, the emergence of the so-called spider veins and reticular veins. The next stage in the development of the disease are: emerging swelling around the ankles, then also swelling of the entire lower leg. Initially the swelling disappears after a night rest, and then becomes constant. After some times varicose veins may occur i.e. permanent extension of superficial veins.
In advanced venous insufficiency of the lower limbs trophic skin changes appear as well as discoloration, spots and hardening. Then itching appears, bumps, cracks, skin covering varicose veins is damaged, which inevitably leads to the formation of difficult to heal wounds known as leg ulcers.
Location
- Typical venous ulcers are located above the medial malleolus leg.
- Ischemic ulcers (arterial) are often found on the back of the toes, on the heel, or on the front surface of the shin.
- Rheumatic ulcers usually involve the side and back surface of the rest of the lower leg and the ankle area.
Where to seek help and advice
Of course, in the first instance go to your GP who should refer you to a specialist surgeon. Currently, the best method of diagnosing venous insufficiency is to perform an Colour Doppler ultrasound test.
Treatment
In case of ulcers resulting from advanced chronic venous insufficiency, leg swelling, not treated varicose veins, it is a standard to conduct a multidirectional model of treatment comprising of:
- local treatment of the wound – treatment by means of dressings,
- compression therapy – treatment with special bandages or stockings,
- drug therapy – treatment with pharmaceuticals – medicines,
- and ultimately the elimination of venous reflux – surgical treatment.
The local treatment is to accelerate the cleansing of the ulcer from necrotic tissue and stimulation of the healing process. The purpose of the conservative treatment is to reverse the effects of venous hypertension, improving venous return, and thus – reducing the swelling. The basis of the conservative treatment is the compression therapy. It increases local hydrostatic pressure and reduces pressure in superficial veins, reducing the transudation of fluid from the blood. Gradual compression accelerates blood flow in the veins of the deep system. An extremely important element of the conservative treatment is the pharmacotherapy.
The treatment of leg ulcers is tough and long-lasting, so to make it the least expensive and effective it must be based on genuine and systematic cooperation with a healthcare professional.
Prevention
Factors which a person can control are WEIGHT and LIFESTYLE.
WEIGHT:
- losing excess weight
LIFESTYLE:
- increasing physical activity especially walking, cycling, swimming. This activities the so-called “calf pump”. Muscle contractions stimulate the venous circulation, pushing blood to the heart – blood does not stop in the veins.
- taking care of yourself in the workplace, especially when staying seated – footrests, avoid staying long in one position without moving or standing. Involving exercises allowing the calf muscles to work – for example, march in place in an upright position, bending towards the foot being in a sitting position.
Once microcirculatory disturbances occur, they can be corrected through the use of compression products:
- knee-socks
- stockings
- anti-varicose tights
and involve medical treatment – always preceded by consultation with your doctor or a pharmacist.
Maria T. Szewczyk, Ph. D.
Department of Surgical Nursing, Ludwik Rydygier Collegium Medicum in Bydgoszcz, Nicolaus Copernicus University in Toruń
In the treatment of ulcers, especially of their advanced form, omnidirectional and interdisciplinary care of the patient is required. Venous ulcers are chronic wounds, where the healing process is difficult and lengthy, and requires the effort of many measures. (…)
Chronic venous insufficiency and venous ulcers
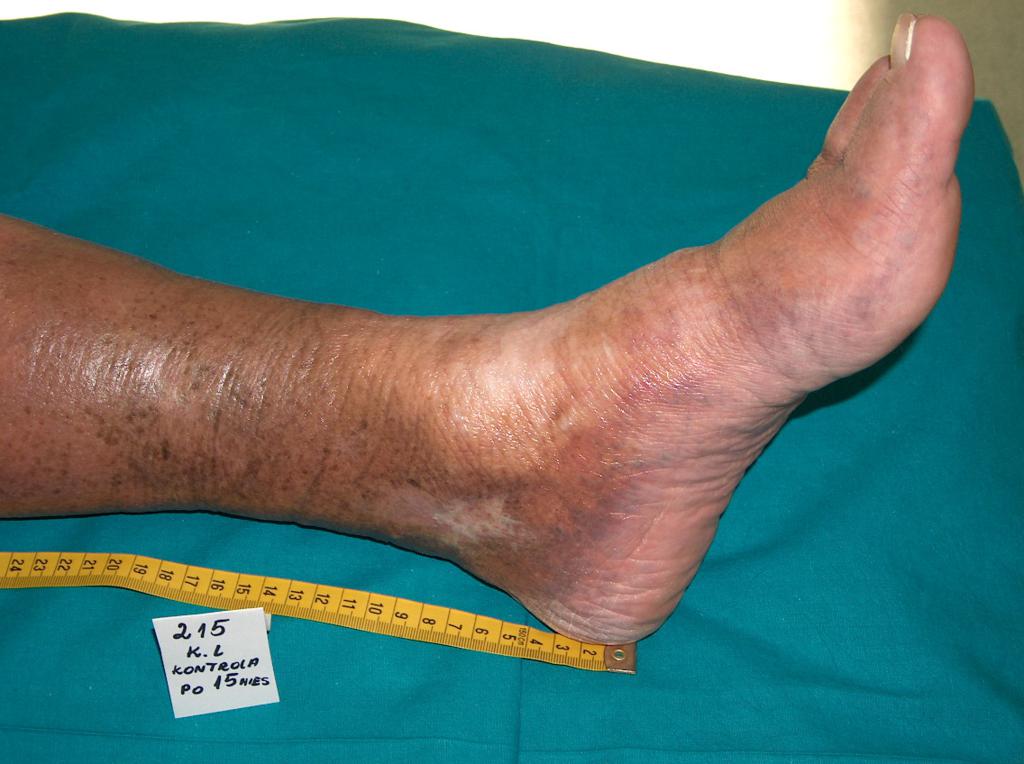
In about 80% of cases the cause of leg ulcers is chronic venous insufficiency. Venous ulcers are the final and most serious complication. In the treatment of ulcers, especially of their advanced form, omnidirectional and interdisciplinary care of the patient is required. Venous ulcers are chronic wounds, where the healing process is difficult and lengthy, and requires the effort of many measures. Extensive and ongoing for years wounds often lead to movement limitation in the ankle joint, foot deformation and permanent disability (Photo 1, 2, 3, 4).
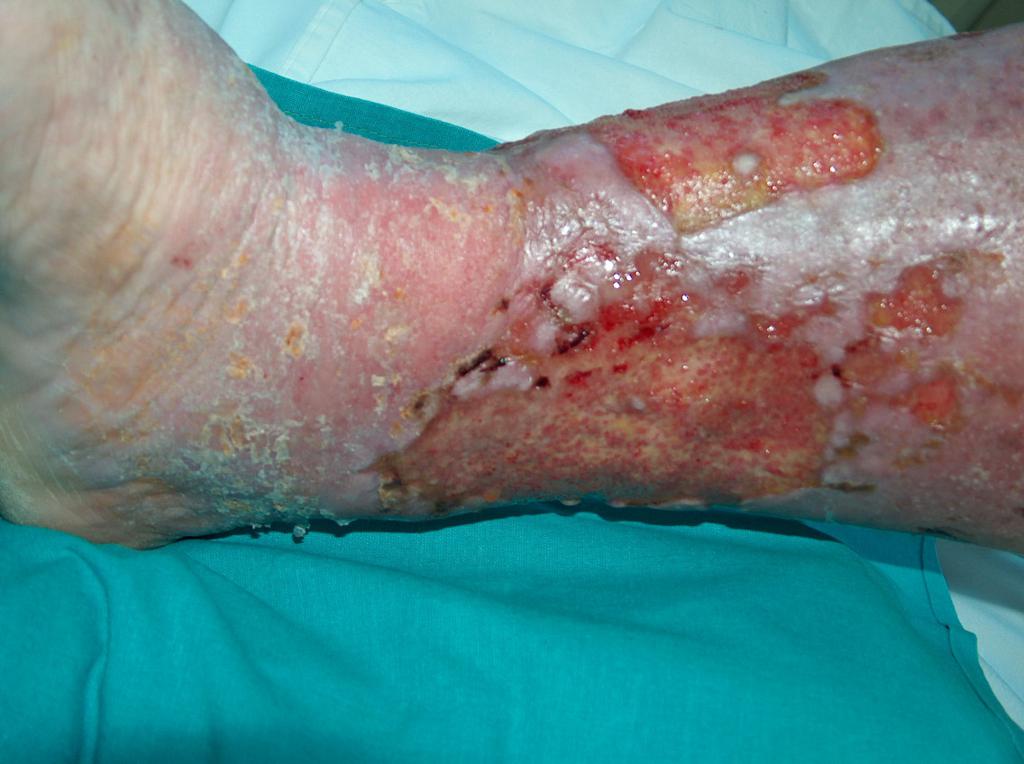
(archive of the author)
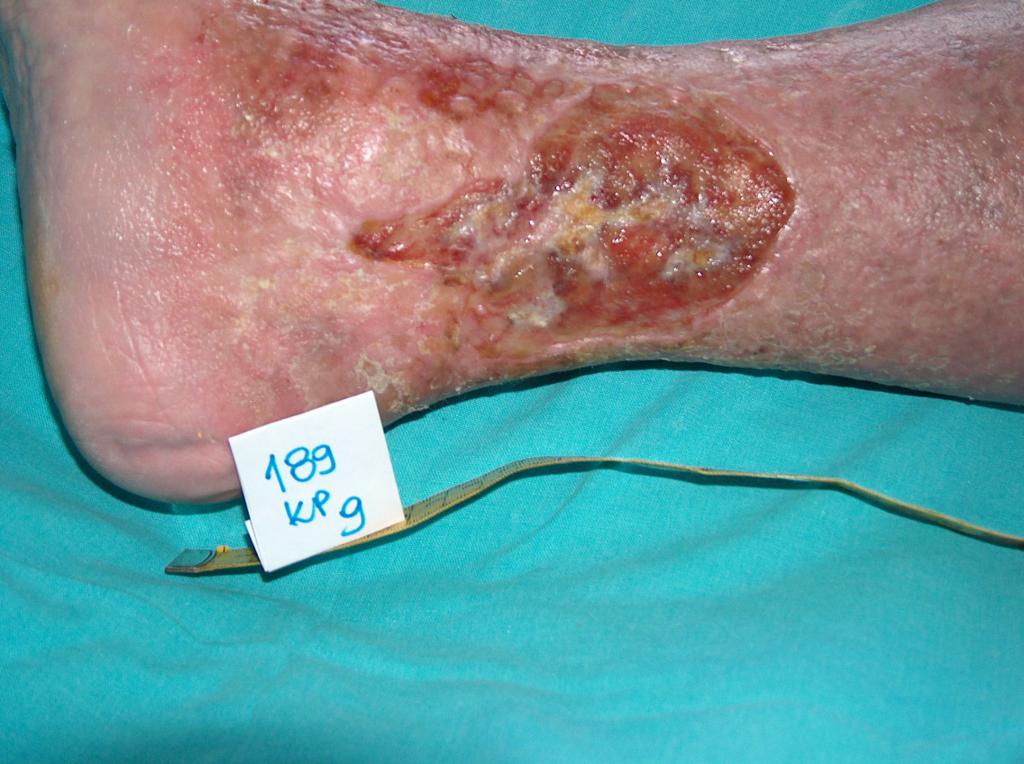
(archive of the author)
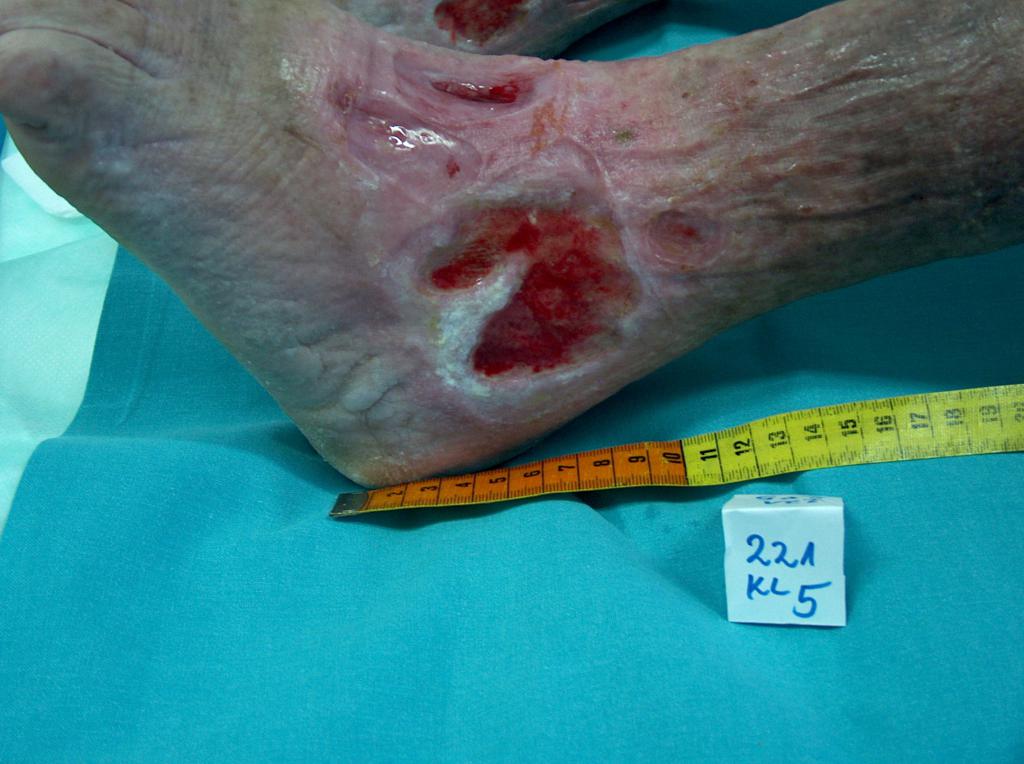
(archive of the author)
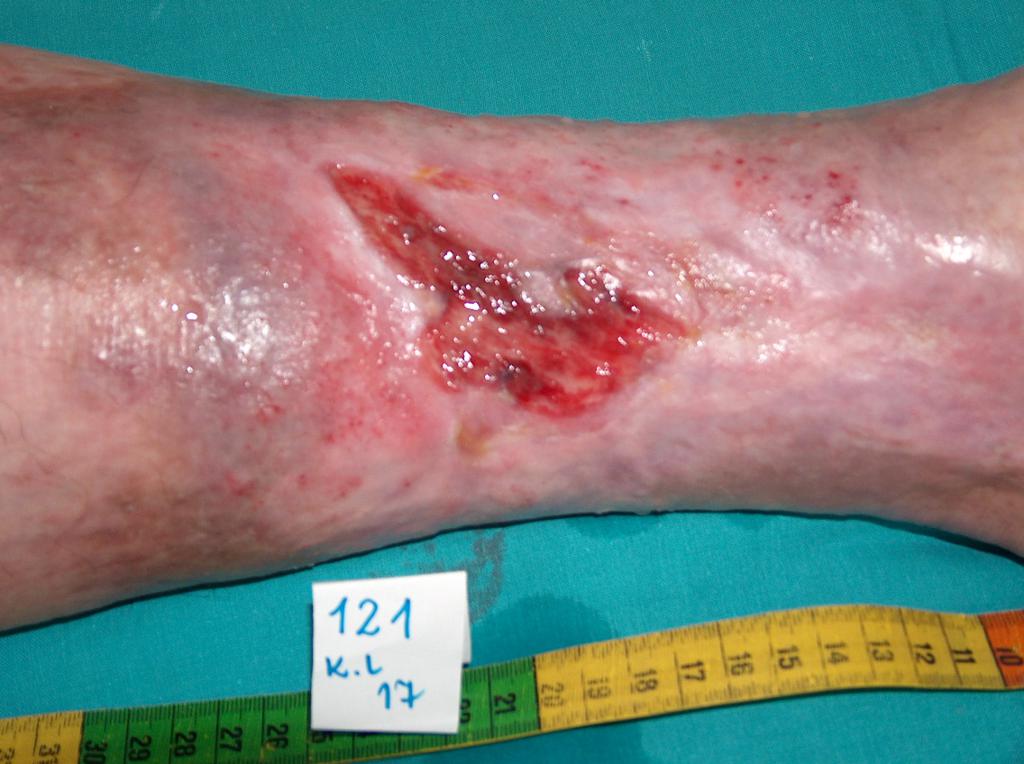
(archive of the author)
The first step is the diagnostic and ultrasound examination of venous vessels, and then topical and causal treatment. Etiopathogenesis, in which the main role plays venous hypertension, requires at first elimination or reduction of causative factors. The cause of ulcers are in fact circulatory disorder leading to the venous hypertension in the lower limbs. These relate to pathological anatomical and physiological changes occurring in several successive stages. It begins with overload and baggy or fusiform enlargement of the vascular system in the form of varicose veins. Accompanying changes include: a decrease of flexibility and patency of blood vessel walls, and valvular regurgitation, venous blood reflex and (or) occlusion of the deep venous system (by e.g. deep vein thrombosis). Long-lasting high hydrostatic pressure eventually leads to an increase in vascular patency and transition – first of exudate and also of cellular components. In the so-called gaiter area of the leg (the lower half of the leg above the ankle and around the ankle) trophic changes occur, initially only in the form of over-pigmentation and discolouration, and later also in the form of inflammation, fibrosis and thinning of the skin tissue. On the surface of these changes ulceration can be developed. The immediate cause of the injury can be not only the changes in the skin nutrition, but also spontaneous rupture of varicose veins, or even a slight mechanical shock.
The gold standard of conservative treatment of venous ulcers is compression therapy followed by wound cleansing and active moist or biological dressings.
Compression therapy
In the conservative treatment a vital role plays compression therapy, which deals with individually chosen compression dressings. It can be bandages (band) with compatible compression degree as well as ready products in the form of knee-length, short and long stockings and tights. The compression therapy using the bandages depends inter alia on the material from which they are made and the method of bandaging the limb. The use of the compression greatly reduces venous hypertension in the superficial system, improves the efficiency of the muscle pump, reduces venous stasis and restores proper hydrostatic conditions for the outflow of blood from the vessels. The compression will be effective if the degree of compression will be applied depending on the severity of chronic venous insufficiency i.e. it will depend on the superficial, perforator and deep vein system. To measure the interfacial pressure of the compression a Kikuhime device is used. With the help of this apparatus we can provide the required pressure. (Photo 5)
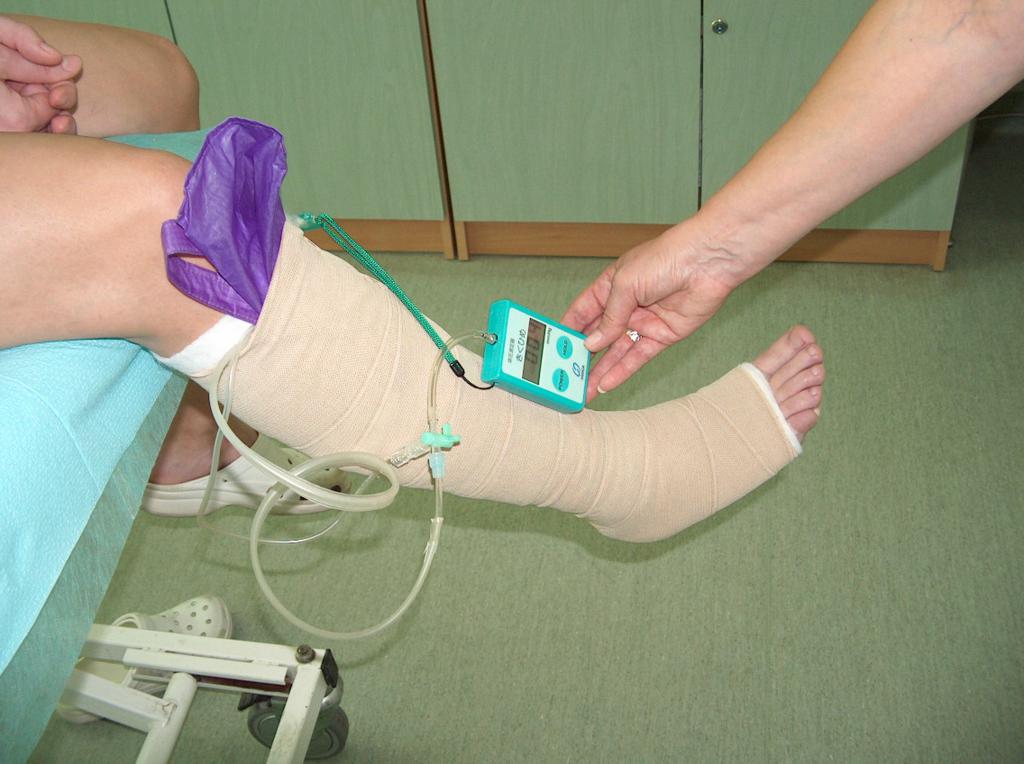
(archive of the author)
Similar effects can be brought by a massage – both sequential pneumatic massage (Photo 6) and manual massage reducing the oedema and improving the return of venous blood towards the heart.
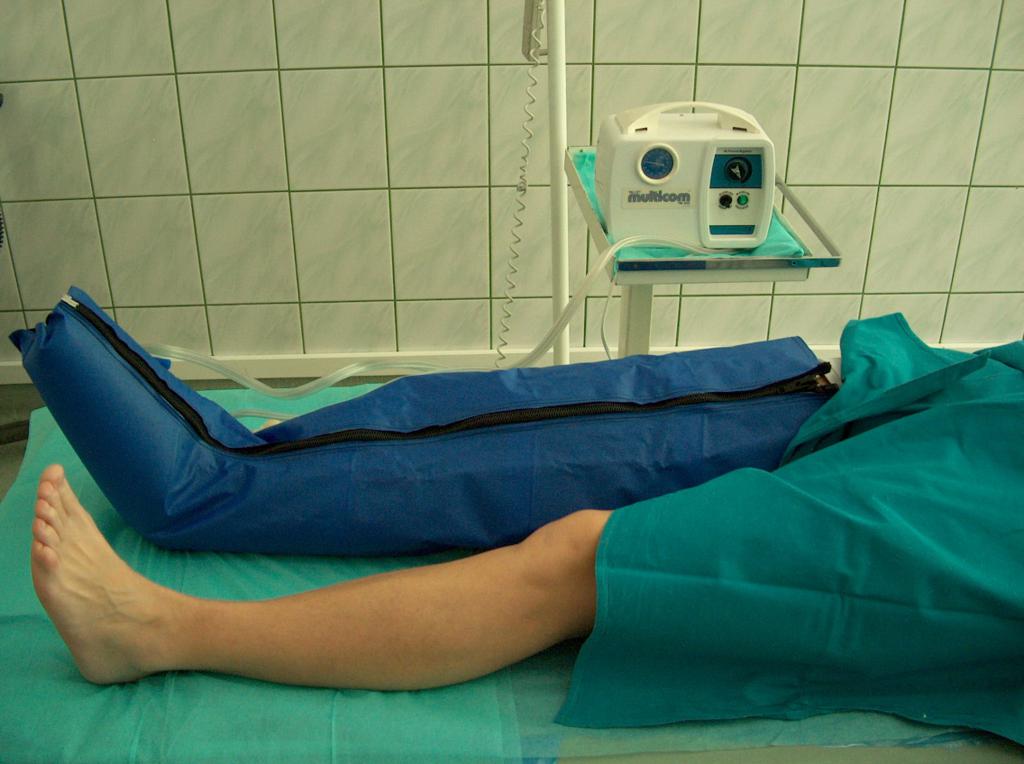
(archive of the author)
Before the use of compression the state of the peripheral circulation must be checked. The use of compression therapy in a patient with impaired blood flow can result in severity of ischemia, skin necrosis, and even limb amputation. Therefore, before applying the compression therapy is necessary to perform Doppler imaging and marking the Ankle Brachial Index (Photo 7).
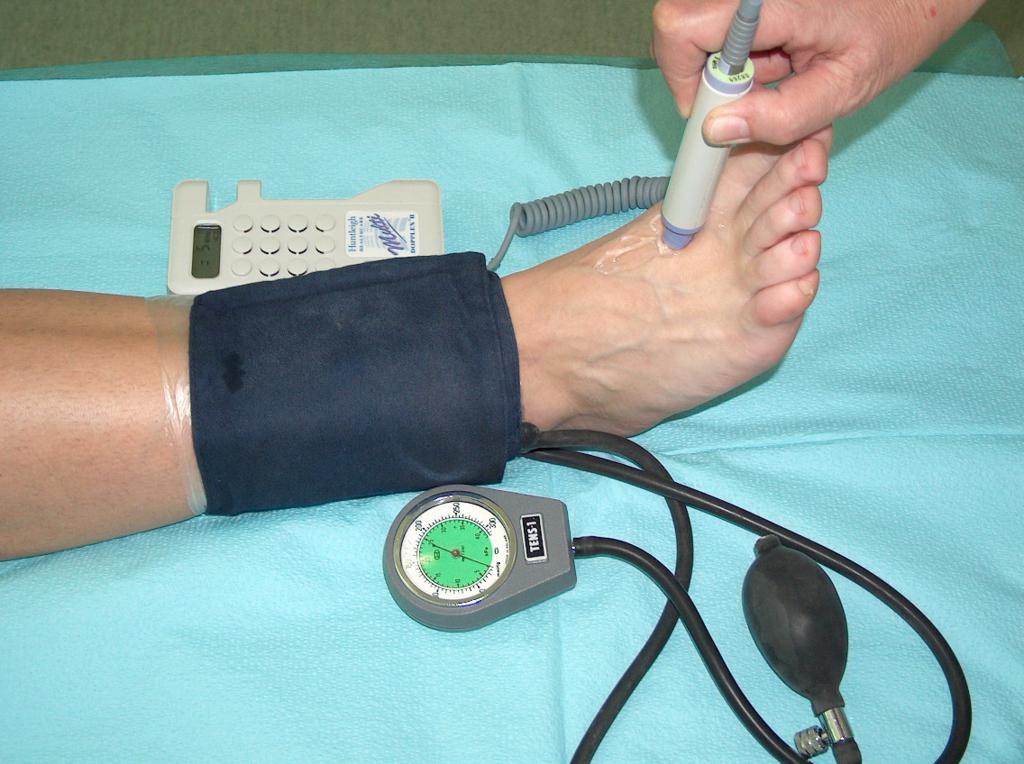
(archive of the author)
Topical proceedings
The topical proceedings parallel with the compression therapy includes: necrosis removal, wound debridement, moist wound healing, care of the skin around the wound.
Contaminations, superficial necrosis reaching the dermis can be removed in a conservative way, e.g. mechanical, enzymatic, autolytic, and in a surgical way. However, necrotic tissues, including subcutaneous layers require a surgical intervention by removal of the changed tissues with a scalpel and scissors. You can also include the VAC system (vacuum-assisted wound closure) as a non-invasive active therapy to promote healing in difficult wounds that fail to respond to established treatment modalities. The method of necrosis removal is determined by the location and depth of the ulcer, the exudate amount in the wound and the patient’s general condition. Of great importance in the selection of the treatment method is the nature and extent of necrosis structures. The mechanical wound debridement, as well as the surgical debridement of wound edges give immediate effect to remove necrotic elements. The autolytic debridement is a natural process that occurs spontaneously in a properly healing wound. It is the effect of proteolytic enzyme and phagocyte activity , which can be both initiated and supported by the maintenance of moist environment at the bottom of the wound. Low severity of these processes in the debridement phase might require to use ready proteolytic enzymes and to introduce enzymatic debridement. Wound cleaning and removal of the necrosis reduces the risk of infection and the development of a local infection. The purpose of this treatment is to prepare the wound to further proliferative processes and stimulation of these processes to maintain optimal healing conditions. Please note that venous ulcers are heavily exposed to the risk of infection. It can be caused by different types of microorganisms (viruses, bacteria and fungi), but the most common etiological agent are bacteria, including staphylococci, streptococci, Escherichia coli and Pseudomonas. Proliferating in the wound, the bacteria secrete its own metabolites and toxins, destroying migrating fibroblasts and budding vessels, and limiting the healing progress. An uncontrolled infection can spread deep inside the wound, infiltrate adjacent tissues, and even lead to the development of sepsis.
The risk of infection and the development of infection can be additionally reduced by flushing the wound bed with antiseptic solution. Its concentration should not only have a bactericidal or bacteriostatic effect, but also should be safe for healthy tissue and does not cause cytotoxic effects or inhibit the healing. Only the preparation meeting the above criteria can be safely applied directly on the wound surface (e.g. Octenisept containing a mixture of octenidyne dihydrochloride and phenoxyethanol safe for skin and mucous membranes). In justified cases general antibiotics are used, which should not be used topically. To support the natural debridement and recovery processes, on a clean wound a special active dressing maintaining moist wound healing environment should be applied.
Moist wound healing
Features of the “ideal” dressing, developed on the basis of Winter analysis (1962) and his successors are satisfied by so-called new generation dressing. They maintain adequate moisture wound environment, which prevents the scab formation and drying out of the ulcer surface. A moist wound heals twice as fast and in a more structured way, because the moist environment stimulates both cell proliferation and the migration of new cells, ensuring their optimal differentiation and neovascularisation.
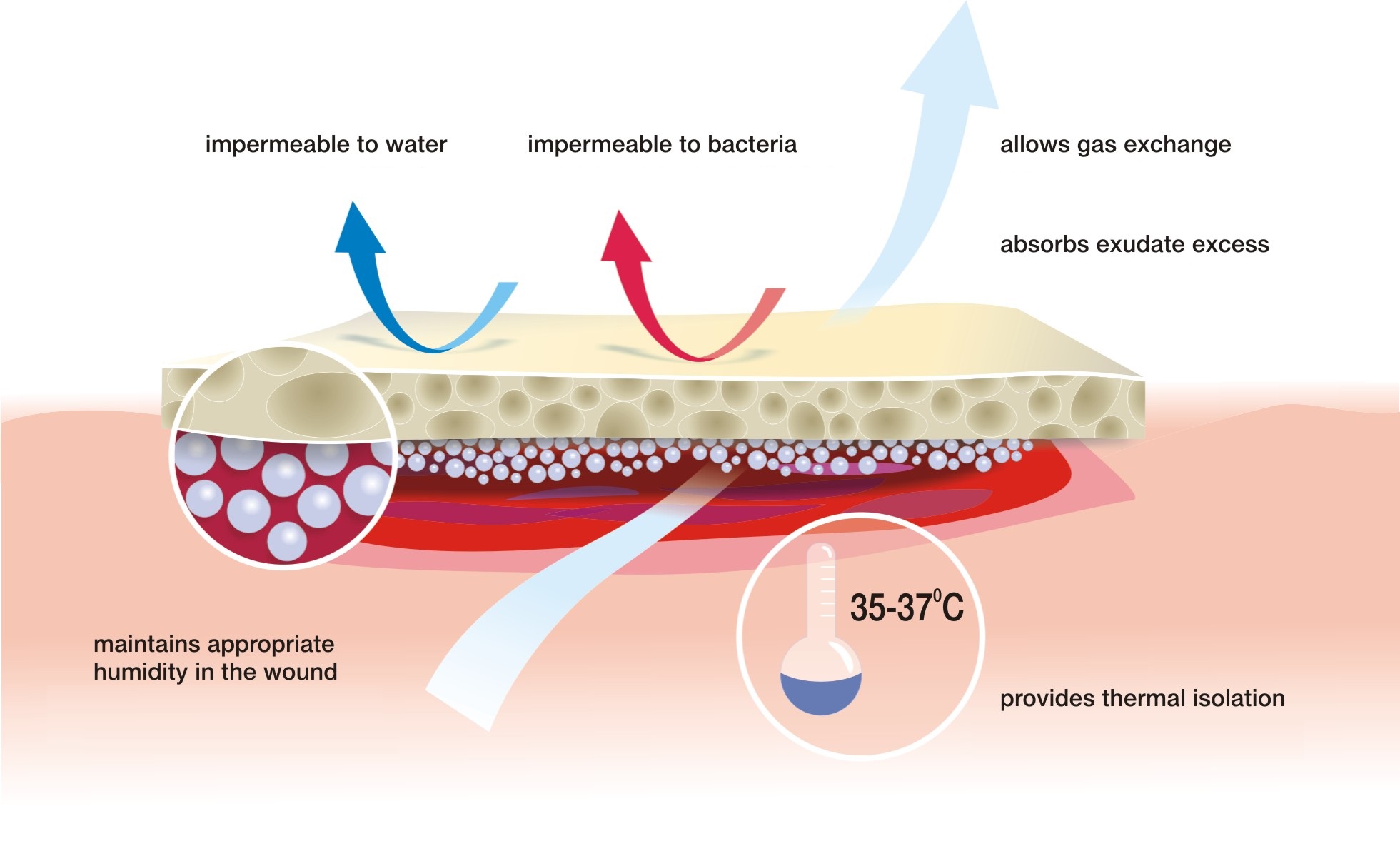
Features of a dressing supporting the natural healing processes were defined in 1991 by Turner et al:
- maintains a moist environment in the wound bed,
- has high absorption capacity, regulates the excess of exudate,
- does not adhere to the wound surface, enables painless and atraumatic change,
- protects the wound against bacteria and contamination,
- is non-toxic and non-allergenic,
- maintains the correct wound temperature similar to the body temperature,
- facilitates the healing process at all wound healing stages.
The new generation dressings fulfilling the listed criteria are produced in several groups, differing in the design and application. They are designed for different types of wounds, depending on their etiology, the healing phase, the depth of tissue damage, the nature of the exudate and the presence of an infection.
The dressings have different properties to keep the exudate, whose secretion varies during the particular wound healing phases. Apart from the outer protection and moisture content control the dressing has to fulfil other important task at every stage of venous ulcers healing.
Skin care
The management of chronic venous insufficiency in states with weak skin barrier function requires particularly attentive care and concentration of efforts aimed at conditioning and regeneration of the natural protective barrier of the epidermis. One of the major care actions taken in concern of the integrity of the skin is to maintain the cleanliness of the body, including the limbs. Cleaning agents used for personal hygiene should be properly chosen and correctly applied, especially when it comes to this group of patients. Detergents are designed to remove and reduce the number of contaminations and microorganisms residing on the surface of the body, if possible without damaging the skin protective barrier. Since the lipid coat has the properties of “binding” impurities, and water alone is not able to overcome them, the washing agent needs to contain surfactants. It is recommended to use agents that are delicate, have a pH of 5.5 or liquid agents containing a substance modifying the acidity of the product (for example: phosphoric acid, citric acid, sodium hydroxide, triethanolamine), and enriched with physiological lipids, ceramides, and moisturising agents, which at least partially allow to compensate for the lipid loss caused by the action of the detergent.
(archive of the author)
After thorough cleaning of the skin it is advised to apply agents supporting the regeneration and increasing the moisture level of the skin. This can be obtained thanks to biologically inert substances supporting the treatment and skin care of the, so-called emollients. Due to moisturising properties, they increase the water content of the stratum corneum and improve the biophysical properties of the epidermis (Photo 8). The emollients are available in form of creams, lotions, ointments and emulsions of different consistency, serving the same purpose – moisturising and / or oiling the dry skin. Creams and ointments usually need to be applied thicker. Agents of lighter consistency, such as lotions, make it possible apply thin film. Agents applied on sensitive skin should not contain alcohol, metals, fragrances, or talc. In specific situations they should contain only water-based hydrophilic ingredients. Distributed on the skin they are easily absorbed, and after washing do not leave unwanted residues.
Literature:
- Benbow M, Burg G, Comacho Martinez F, et al. Guidelines for the outpatient treatment of chronic wound and burn. Blackwell Science, Berlin-Vienna 1999, 12-21.
- Szewczyk MT, Jawień A.: Chosen aspects of conservative treatment of venous ulcers. Part I: Compression therapy. Progress Dermatol. Alergol. 2005, XXII, 3: 133-140.
- Blair S, Wright D, Blachkouse C, et al. Sustained compression and healing of chronic venous Ulcers. Br Med J 1998, 298: 1159-1161.
- Ciecierski M, Jawień A. Clinical picture of chronic venous insufficiency. Medical guide 2004, 8 (68): 36-48.
- Hess CT. When to use hydrocolloid dressing. Nursing 1999; 29.11: 20-23.
- Szewczyk MT, Jawień A, Piotrowicz R. Treatment of venous ulcers. Medical guide 2004, 8 (68): 66-71.
- Szewczyk MT, Jawień A, Piotrowicz R. The use of compression therapy in venous diseases. Medical guide 2004, 8 (68): 58-64.
- Jawień A. Szewczyk MT. (red) Venous leg ulcers. Ed. Your Health. 2005.
- Jawień A. Szewczyk MT. (red) Clinical and nursing aspects of care for patients with venous ulcers. Termedia 2008.
- Szewczyk MT., Mościcka P., Cwajda J. et al Evaluation of the effectiveness of new polyurethane foam dressing in the treatment of heavily exudative venous Ulcers. Acta Angiol. 2007 T.13, 2: 85-93.
- Placek W. Role of substrates and emollients in the prevention and restoration of the epidermal barrier. Aesthetic Dermatology 1999, 4: 174-178.
- Korinko A. Yurick A. Maintaining skin integrity Am J Nurs 1997 (2): 40-44.
- Wojnowska D., Chodorowska G., Juszkiewicz-Borowiec M. Dry skin – pathogenesis, clinic and treatment. Advances in Dermatology and Allergology, 2003, XX, 2: 98-105.
- Szewczyk MT, Jawień A. Recommendations of specialised nursing care of patients with venous leg ulcers. Surgical and Vascular Nursing 2007, 3 (1): 95-129.
Causes
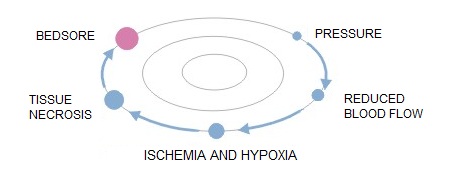
The cause of pressure ulcers (also called bedsores, decubitus ulcers or pressure sores) is tissue ischemia due to the prolonged pressure evoked on veins and arteries.
The risk of pressure ulcers depends on the duration of the pressure – the longer the pressure is present or the greater the force, the greater the possibility of developing bedsores.
In healthy people prolonged pressure causes pain forced to change position.
Unconscious and immobile people are not able to relieve the pressure automatically and to improve the blood circulation, thus they belong to the group of people at increased risk of pressure ulcer development.
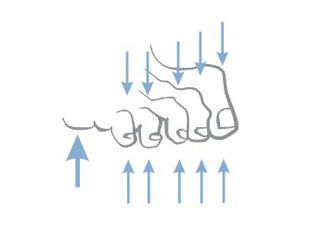
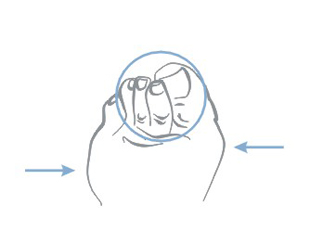
Pathomechanism of developing bedsores:
- simple pressure i.e. the pressure exerted on the soft tissue on one side by the bone, and on the other by a hard surface
- rubbing the patient’s body surface over bed linen e.g. when using improper technique for changing positions
- lateral tensile forces, which act directly on the patient’s body
Risk group
The risk of developing pressure ulcers should be considered in all patients with long-term reduction of capacity for self-movement, which spend most of their time in bed or in a wheelchair.
Factors that increase the risk of pressure ulcer development are:
- age
- weight
- nutritional status
- sphincter function of the urethra and the anus
- state of consciousness
- diabetes, atherosclerosis
- steroid therapy
Symptoms
Pressure ulcers are classified according to the severity of the symptoms into 4 or 5 degrees. And hence:
- Stage I: intact skin with non-blanchable redness of a localised area usually over a bony prominence. The area may be painful, firm, soft, warmer or cooler as compared to adjacent tissue. Microcirculation is not damaged yet.
- Stage II: partial thickness loss of dermis presenting as a shallow open ulcer with a red pink wound bed, without slough. Presents as a shiny or dry shallow ulcer without slough or bruising.
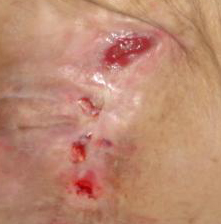
- Stage III: abrasions, cracking skin and full-thickness skin damage to the border of the subcutaneous tissue, blisters, the wound edges are well marked out, surrounded by edema and erythema
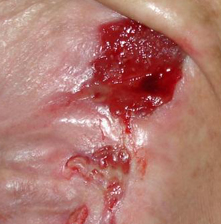
- Stage IV: the damage extends towards the subcutaneous fatty tissue; the ulceration can be free from infection and necrosis and covered with clear granulation tissue, but the necrosis may also affect the fatty tissue and the surrounding skin layers. The bottom may be covered with black necrosis.
- Stage V: the presence of advanced necrosis, which extends towards the fascia and muscles; the damage can also affect joints and bones – unpleasant odour and profuse pus-necrotic discharge; in the wound there are pieces black dead tissue and black necrosis
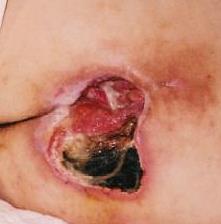
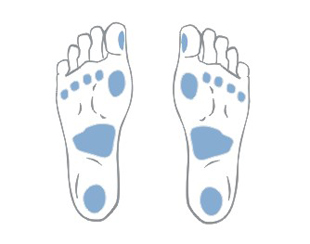
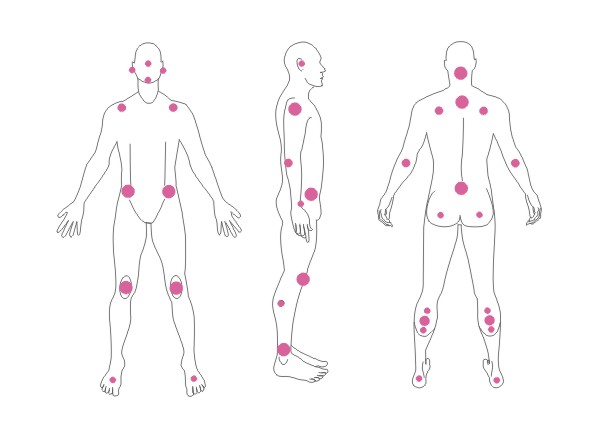
Location
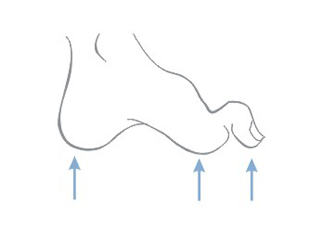
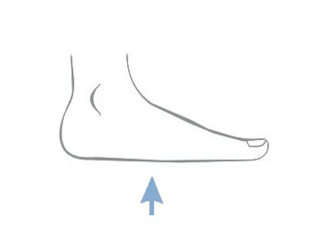
Bedsores occur in places where the distance between bone prominence and the skin surface is the smallest i.e. in contact point of the skin and the ground, where the pressure is the highest. Most pressure ulcers are formed around the aitchbone, coccyx, buttocks, on the heels or the hips.
The above figures present the point of contact of the skin with the surface at various positions of the patient laying on the bed.
Where to seek help and advice
Of course, in the first place consult the general practitioner.
The treatment of pressure ulcers is the responsibility of a doctor and a nurse who has completed a specialist course in the treatment of chronic wounds. The competences of nurses are limited to the treatment of pressure 1 to 3 degree sores.
Sometimes the condition of the wound requires surgical debridement and then the GP directs us to a specialist surgeon.
The treatment of pressure ulcers is tough and long-lasting so to make it the least expensive and effective it must be based on genuine and systematic cooperation of the doctor and the patient, and must be combined with an intensive, professional care.
Treatment
First of all the treatment should be conducted under the supervision of a doctor or a nurse.
Bedsores are treated locally i.e. the wound is to be secured with dressings appropriate.
A very important part of treatment is also appropriate patient care, which include:
- position changing – the patient should not lie on the bedsore
- placing patient on a pressure relief mattress
- protecting sore places with special anti-bedsore discs and stands
- adequate nutrition and hydration of the patient
- controlling comorbidities
The most effective form of treatment is the use of specially designed wound dressings for this purpose, the so-called specialised or advanced dressings that create a moist wound healing environment.
Choosing the right, effective dressing it must be based on a correct diagnosis of the processes occurring in the wound. To make it easier, you can use the wound colour classification matrix, which is based on the observation of the phenomena that take place in different phases of healing.
Wound colour classification matrix:
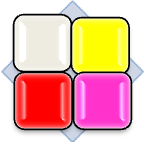
Black wounds
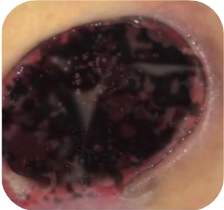
Wounds with black necrosis require:
- maintaining a moist environment
- removal of necrotic tissue in order to initiate the healing process
The healing process will not occur under thick layers of necrotic tissue; to begin it first the necrosis needs to be removed. We have a choice of two basic ways to get rid of the necrosis from the wound bed:
- surgical debridement – the mechanical removal of necrotic tissue to expose healthy skin structures for initiating the process of wound healing
- application of interactive dressings – involves the application of dressing on a wound, which stimulates the autolysis process i.e. the natural wound cleansing by the body. In this case the necrosis decomposition is made by enzymes produced by the damaged wound cells.
Recommended dressings for black wounds:
- Medisorb G – hydrogel dressing
Yellow wounds
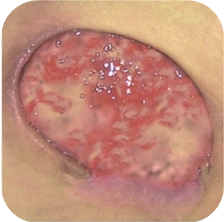
Wounds with yellow, colliquative necrotic tissue require:
- maintaining a moist environment
- absorbing excess exudate, along with the remnants of necrotic material
Wounds with colliquative necrosis are characterised by an increased exuding level. The necrosis on the bottom of the wound is liquid. Such wounds provide an ideal environment for the growth of microorganisms, and therefore they are often infected. The tasks for the dressing in this case is the absorption of exudate and necrotic material, liquefaction of too dry and too dense necrosis, protection against drying out and against secondary injuries.
Recommended dressings for yellow wounds (depending on the exudate level and the depth of the wound):
Medisorb A – alginate dressing – heavy or moderate exuding wounds; superficial and deep wounds
Medisorb P – absorbent dressing – heavy or moderate exuding wounds; superficial wounds
Medisorb H – hydrocolloid dressing – moderate and low exuding wounds; superficial wounds
Red wounds
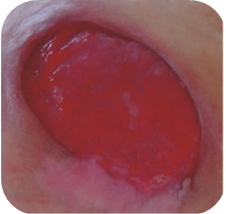
Red wounds with visible granulation tissue required:
- maintaining a moist environment
- protecting against secondary infections
- controlling the exudate level
Apart from maintaining a moist environment, these wounds also require protection against possible mechanical injuries. This is particularly important since a well-vascularised granulation tissue is susceptible to injuries which delay the healing process and can be the source of infection. Another important factor is to maintain the proper temperature (close to body temperature), so that new cells can grow at optimum speed.
Recommended dressings for red wounds (depending on the exudate level and the depth of the wound):
- Medisorb A – alginate dressing – heavy or moderate exuding wounds; superficial and deep wounds
- Medisorb P – absorbent dressing – heavy or moderate exuding wounds; superficial wounds
- Medisorb H – hydrocolloid dressing – moderate and low exuding wounds; superficial wounds
Pink wounds
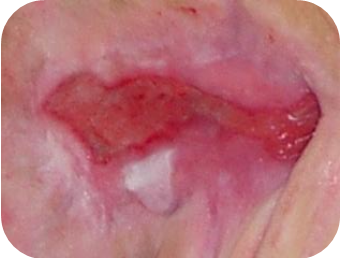
Pink epithelising wounds require:
- maintaining a moist environment
- protecting sensitive tissues
When the wound begins to cover with epidermis it needs to be protected against drying out, friction and other factors that could damage the newly formed tissue.
Recommended dressings for pink wounds (depending on the exudate level and the depth of the wound):
- Medisorb H – hydrocolloid dressing – moderate and low exuding wounds; superficial wounds
- Medisorb F – film dressing – low exuding wounds
The analysis of wound healing phases shows that wounds being at various stages of healing, require some other conditions for the process to run smoothly. It is important to remember that in addition to various healing stages, the wounds are also varied because of the size, depth, presence of necrotic tissue and exudate level. All these features result in the fact that each wound requires the selection of the right kind of dressing, sometimes even a few dressings that will change during the healing process.
The following table presents factors that may slow down the healing process.
Table: Factors slowing down the wound healing process
| slowing down factor | why | optimum conditions | how does it work in optimum conditions |
| dry environment | moist environment | appropriate level of wound exudate: allows activation of natural wound debridement; accelerates granulation; provides quick and correct course of epithelisation | |
| necrotic tissues | wound healing is possible only after the removal of dead tissues; the necrosis may be a substrate for the development of infection | curgical / autolytic wound cleansing | cleansed the wound enable the begin of the granulation phase |
| infection | all mechanisms in the wound tend to fight the intruder; the healing process is hampered | fight infection | cleansed the wound enable the begin of the wound healing process |
Prevention
Basic rules:
- systematic change of body position every two hours and reduce pressure in places at risk, through the use of special pressure relief mattresses and pads
- adequate nutrition and hydration
- protect the skin by the use of additional breathing aids – diapers, special protective dressings – polyurethane film dressing and appropriate skin care products
- documentation of symptoms and changes in body position
Renata Kobierska
Director of the Nursing Home in Kalisz
Types of diabetes
Diabetes is a result of lack of insulin (a hormone produced by the pancreas) in the body. The role of insulin is comparable to the role of the key – thanks to it we get into the apartment, and thanks to insulin sugar (glucose) can get into the body’s cells where it is converted among other things into energy. If there is lack of insulin in the body, sugar builds up in the bloodstream.
Currently, there are two prevalent types of diabetes: type 1 and type 2. The causes of this condition are different depending on the type of the disease.
Type 1 diabetes, formerly insulin dependent diabetes or juvenile diabetes, is caused by a complete lack of insulin due to the damage of appropriate cells of the pancreas. It occurs mainly in children and adolescents, hence its name. The emergence of the disease is not fully known. We only know that it is genetically determined, resulting in impaired immune mechanism and further in damage to the beta cells of the pancreas.
Type 2 diabetes, formerly noninsulin-dependent diabetes, is the most common form of the disease. The cause is usually impaired insulin secretion by pancreatic beta cells or the use of insulin by tissues. This diabetes occurs most often in the elderly people, obese, or with other metabolic disorders. In the early stage of the disease insulin is secreted in increased amounts, but at the same time the amount is insufficient for the increased needs of the body (insulin resistance).
In the literature there are many definitions of diabetes, and one of them says that it is a group of various genetically determined and acquired metabolic disorders that are characterised by glucose intolerance and hyperglycaemia, and over time the emergence in the vascular system, nervous system and other organs of changes referred to as chronic complications of diabetes. The cause of impaired glucose tolerance is the lack of insulin or its inappropriate tissue action. The name “diabetes” according to the new classification means a disease with a complete clinical picture, and mild carbohydrate metabolism disorders are called impaired glucose tolerance. 1
However, according to J. Tatoń diabetes is “a large group of diseases and metabolic disorders of various etiology, characterised by a constant, pathological fasting hyperglycaemia, between meals or just after a meal, resulting from the failure of insulin secretion by pancreatic beta cells or impaired response of cells, tissues and peripheral organs”. 2
In 1997 the American Diabetes Association developed a new division of diabetes, which was modified in 2003 and is now it looks as follows:
- type 1 diabetes – the destruction of beta cells leading to absolute insulin deficiency
- type 2 diabetes – a progressive disorder of insulin secretion and insulin resistance
- other specific types of diabetes – caused by genetic defects of beta cell function and insulin action, by exocrine pancreatic diseases, certain drugs or chemicals
- gestational diabetes – diagnosed during pregnancy
Classification of type 2 diabetes by Tatoń:
1. Genetic conditioning:
- occurring within a family
- with the occurrence of erythema after chlorpropamide and alcohol
- associated with syndromes caused by genetic disorders
- type 2 diabetes syndrome in young people
2. Nutrition conditioning:
- hyperplastic obesity
- hypertrophic obesity
- without obesity
3. Determinants of disturbed cell reactivity to insulin:
- with an excess of hormonal “anti-insulin” factors
- with impaired insulin receptor function
Each of these subtypes can be divided into type 2 diabetes treated with:
- diet alone
- oral hypoglycaemic medicines
- insulin 3
Symptoms
Type 2 diabetes has often latent asymptomatic course, so it cannot give characteristic symptoms. This disease is like a “mask” and as a result it is often diagnosed only when symptoms get worse or when another illness appears. The “mask” symptoms characteristic for type 2 diabetes include:
- skin symptoms – itchy skin, especially in the genital area, boils, thrush, fungal nail infections, poor wound healing, xanthomas, hair loss
- gynaecological symptoms – vaginal bacterial infection, vaginal thrush, menstrual disorders, impotence
- nervous system symptoms – numbness, stinging, burning, loss of sensation – especially in fingers and toes, nocturnal leg cramps, weakness of one of the nerves
- fatigue, weakness
- blurred vision
- miscarriages

The typical symptoms of type 2 diabetes include:
- general weakness
- increased thirst
- increased appetite
- thinning
- polyuria
- infections
- skin inflammation and itching 4
Every cell in our body need glucose i.e. sugar, which is the source of energy and affects the normal functioning of the brain, muscles, liver, kidney and heart. The glucose to penetrate into the cells requires insulin. When cells become resistant to the hormone, the sugar cannot get into them, but circulates in the bloodstream. This causes an excessive amount of glucose in the blood (hyperglycaemia) and so-called cell hunger. The body in defending itself from the lack of sugar triggers the mechanisms of increased appetite, but due to the lack of insulin the glucose from food cannot get into the tissues – is excreted in the urine. Undiagnosed type 2 diabetes leads to severe complications. Can cause atherosclerosis, heart attack or stroke i.e. conditions associated with the damage to large blood vessels. The second type of complications results from the damage to small blood vessels. These include, inter alia, retinopathy (eye disease), which can lead to blindness. Patients may also suffer from kidney failure and circulatory disorders and innervation of the lower limbs. They lead to the development of so-called diabetic foot ulcers – wounds and ulcers occurring on the leg. If this condition is not healed in time it may lead to amputation.
How to live with diabetes
It is possible to live a normal life with diabetes provided that a few basic rules are obeyed:
- education i.e. consciousness – in diabetes, as in any other disease, the patients are responsible for their own health
- nutrition – drug therapy with appropriate diet does not differ from the one recommended for healthy people
- physical exercise – walking, playing sports should become a habit, because it provides good physical form of every human being
- medicines – modern treatment consists of therapy that allows to restore similar processes that take place in the body of a healthy man
Literature:
1. A. Czyżyk, Encyklopedia chorego na cukrzycę, PWN, Warszawa 1992.
2. J. Tatoń, Poradnik dla osób z cukrzycą typu 2, PZWL, Warszawa 2002.
3. J. Tatoń, Diabetologia kliniczna, PZWL , Warszawa 1986.
4. P. Hien, Cukrzyca, krótki kurs diabetologii, Sprinter, PWN, Warszawa, 1997.
Jolanta Machańska
Educator in Diabetes
Diabetes is a major and increasing health problem. It affects people at any age and in all countries. It is a disease that lasts from its inception throughout the patient’s life, usually for a few dozen years.
It is one of the main direct and indirect perpetrators of disability – blindness, kidney failure, gangrene and amputation of the lower limbs, the severity of coronary heart disease and stroke and early human mortality.

Complications of diabetes can be acute i.e. states where deep metabolic disorders appears suddenly, usually combined with disorders of fluid-electrolyte balance and acid-alkaline balance, fast leading to a significant impairment of general condition, loss of consciousness and sometimes death.
The second group of complications are chronic diseases i.e. specific groups of disorders and symptoms of being a clinical exponent of changes in vessels, nerves and other organs that appear along diabetes and contribute to disability and premature mortality.
ACUTE COMPLICATIONS
Acute metabolic disorders – diabetic comas, in fact, is not a complication of diabetes, but the consequence of insulin deficiency. In the period before the discovery of insulin they were regarded as the final stage of the disease. Currently they appear only if there is no or improper treatment. Diabetic coma can have a different course, which results from separate pathogenic mechanisms leading to this condition.
At this time, the following types are distinguished:
- diabetic ketoacidosis
- severe diabetic hypoglycaemia
- hyperosmolar nonketotic coma
Diabetic ketoacidosis
Occurs most often (mainly in patients with type 1 diabetes – juvenile diabetes, absolute insulin deficiency) and the best known. It develops in the course of diabetic ketoacidosis, which affects mainly people completely devoid of pancreatic islet beta cells.
Causes:
- infections, especially purulent ones where rapidly increasing insulin resistance results in increased demand for insulin
- severe systemic diseases such as myocardial infarction, stroke, pneumonia, and major surgeries
- pregnancy with insulin resistance and increased insulin demand
- lack of patient education – often ignorant patients discontinue insulin delivery due to the loss of appetite (fever) and fear of hypoglycaemia
The clinical picture is quite diverse, and the intensity and type of common ailments and symptoms are not always formed parallel to the results of laboratory tests.
Symptoms may be presented in several groups:
Consequences of dehydration: very large thirst, polyuria reaching a few litres a day, dry tongue and mucous membranes, dry skin, soft eyeballs. Initially there is an increase in body temperature, which, if there is no infection, later turns into hypothermia, a drop in blood pressure, especially in elderly people, in extreme cases, loss of pulse and bruising of the distal parts of the body.
Gastrointestinal disorders: dreg type vomiting, abdominal pain – in extreme cases, false peritoneal symptoms (ketotic abdomen), enlargement of the liver.
Respiratory disorders: Kussmaul breath (breath of a chased dog) – deep and laboured characterised by four phases: inhale – pause – exhale – pause, acetone odour can be felt in the breath – the smell of rotten apples.
Consciousness disorders: four stages can de distinguished in the developing ketoacidosis:
- tiredness, impaired balance and vision
- state of somnolence, abnormal thinking
- deep sleep with preserved reactions to painful stimuli: the weakening of physiological reflexes
- deep neurological coma with the reduction of response to painful stimuli and physiological reflexes
Treatment
Once the diabetic coma or being at risk of it is diagnosed, the patient should be immediately sent to the nearest hospital. It would be perfect if there was diabetes ward with intensive care room in the hospital.
The treatment of diabetic ketoacidosis includes:
- insulin delivery – preferably by continuous infusion by means of a pump
- supplementing fluid and electrolyte insufficiency
- use of alkalising medicines
- treatment of complications
Hypoglycaemia
Another condition which is a complication not of diabetes itself, but the treatment. Blood hypoglycaemia of various severity are the most common complications arising in people treated with insulin; therefore, anyone who comes into contact with diabetics, should have knowledge about hypoglycaemia.
Causes:
- errors in insulin therapy: determining too much insulin, a mistake in the measurement of the dose of insulin, too late reduction of the dosage, when patient’s body weight decreased, diet therapy proved to be more accurate, infection was removed
- the pursuit of too rapid metabolic levelling out by a large increase in the dose of rapid-acting insulin, or despite the absence of conditions for this
- errors in nutrition: too long intervals between meals, too little carbohydrate in the meal, alcohol
- disorders of the gastrointestinal tract: vomiting, diarrhoea, abnormal gastric emptying
- changes in the absorption of insulin: change of injection place, the muscles in the thigh, where insulin is administered (march immediately after the administration of insulin), heating the injection site (shower after the injection), change in the depth of the puncture, accidental intramuscular or intravenous injection
- starting a new vial of insulin: the insulin may be more active than previously used, stored at room temperature
- reduced need for insulin due to emotional hyperactivity, menstruation, hormonal disorders
- intake of glucose lowering medicines: acetylsalicylic acid, beta-blockers
- increased physical activity
- natural remission of diabetes
Signs and symptoms:
There are many symptoms of hypoglycaemia. Particularly rich and varied individually is the subjective symptomatology. Symptoms are more limited objective and non-specific. Time and rate of increase of symptoms depend to a large extent on the type of insulin, the amount of injected dose and the daily dosage schedule.
In blood hypoglycaemia we can distinguish:
Neurovegetative symptoms (catecholamine): agitation, fatigue, skin pallor, sweating, dilated pupils, tachycardia, a moderate increase in pressure. Symptoms present at glucose concentration of 65 – 55 mg/dl.
Neuroglycopenia symptoms are caused by a reduction of transmission of glucose to the brain. They can be divided into mental symptoms: anxiety, abnormal thinking, cognitive disorders, inability to concentrate, personality changes, amnesia, manic behaviour, delirium, and neurological symptoms: slurred speech, vision, clonic and tonic spasms, overactive tendon reflexes, positive Babinski sign, loss of consciousness. These symptoms occur when the glucose concentration reached approximately 45 mg/dl.
The neurovegetative symptoms are a warning to the patient of threatening neuroglycopenia and are indication for acute prophylactic – eating a meal or sugar. Within time these symptoms of diabetes are reduced or even disappear.
Treatment
The treatment deals with immediate administration of carbohydrate in an amount increasing blood glucose. Mild hypoglycaemic states are treated by the consumption of additional food, if necessary, a few lumps of sugar that a diabetic patient should always have on him/her.
In states of unconsciousness 1 mg of glucagon should be injected. Upon regaining the consciousness, the patient should be fed and watered with sweet liquid until return to normal glucose level. If we are able to give drugs intravenously, the patient should get 1 mg of glucagon subcutaneously, then we give 5 or 10% glucose until the glycaemic stabilises. In case of insulin overdose, after transient improvement the hypoglycaemia may occur again. Such a patient requires hospitalisation. In most cases of hypoglycaemia the prognosis is good. It can be quickly and easily controlled. However, repeated hypoglycaemic states can cause chronic threat due to the extinction of warning signs and abnormal neurohormonal regulation of glycaemic homeostasis.
Very severe hypoglycaemic shock can lead to death or cause permanent damage to the central nervous system and permanent maintenance of mental and neurological symptoms. In diabetic patients treated with insulin, the appearance of hypoglycaemia state is an alarming condition and requires prompt clarification of the cause of this complication, and if necessary correction of the treatment. Appropriate therapeutic programs should implement, taking into account the patient’s involvement in order to minimise the risk of this complications.
CHRONIC COMPLICATIONS OF DIABETES
The characteristic feature of organ changes, referred to as chronic complications of diabetes, is their slow and long-term development. Therefore, they disclose as well-defined clinical syndromes or less specific symptoms of the disease at a later stage, and only then they can cause disability and life threat. For these reasons they are called late complications of diabetes. Long-term asymptomatic evolution of the changes bears the danger of underestimating the negative impact on the prognosis of diabetes.
The major chronic complications of diabetes include:
- changes in the vessels – angiopathia diabetica, changes affect both large vessels – macroangiopathy, and small vessels and capillaries – microangiopathy
- changes in peripheral nerves – neuropathy
- changes outside the circulatory and nervous system: gastrointestinal tract, skin, motor organ, lens
Microangiopathy
Small vessel disease are diabetes-specific changes in the capillaries, which are present in all organs, in which the vessels have a basal membrane e.g. changes to the capillaries in the eyes and kidneys cause such significant damage to these organs that it is disclosed in the form of characteristic clinical syndromes. These syndromes are the cause of disability, and even premature death.
Treatment
The treatment should be initiated by the correction and providing the best possible clinical and biochemical indicators. It is important to introduce the change relatively slowly. Too violent attempts to stabilise the diabetes may lead to accelerate the progress of changes. In the symptomatic treatment vessel sealing preparations are used.
Prevention refers to optimal diabetes treatment from the beginning of the disease with the use of contemporary therapies. It is recommended to take early prevention in form of regular evaluation of the ocular fundus and kidney function.
Macroangiopathy
Large vessel disease whose anatomical substrate is atherosclerosis, and to a lower extent – hardening of arterioles. Changes in the arteries and arterioles are very common in diabetes and appear earlier and are more intensive, which in turn causes premature death or disability. They are especially common among patients with type 2 diabetes, especially in the elderly.
Characteristic features of the large vessel disease in people with diabetes:
Coronary heart disease is most common and is the leading cause of death in diabetic patients. A characteristic feature is asymptomatic and painless myocardial infarction. Approximately in 8% of people with diabetes, both women and men, an ECG test shows abnormalities that might be the evidence of past cardiac necrosis. This applies mainly to patients with long-lasting diabetes, in whom coronary artery disease coexists with other late complications of diabetes, especially diabetic nephropathy.
Cerebrovascular disease is a collection of non-specific for diabetes neurological syndromes, which are the clinical expression of brain ischemia as a result of atherosclerosis and hardening of the arterioles. Cerebral haemorrhages rarely occur in diabetic patients. Thromboembolic changes prevail, which can cause cerebral infarction and softening. Approximately in half of the diabetic patients after stroke also microangiopathic, retinopathic and nephropathic changes appear.
Leg artery disease is the equivalent of arterial occlusive atherosclerosis. The name “leg artery disease” was introduced the WHO Expert Committee on Diabetes to note that:
- vessel changes in diabetic patients are more varied and apart from the atherosclerosis of large vessels include also the sclerosis of arterioles and small vessel disease, and therefore are more extensive and reach the end of the limb
- in diabetes the changes in a specific way focus in the lower limbs; the changes are here more advanced than in other sections of the vascular system.
Occlusion of bigger arteries or arterioles by a sudden or more slowly forming clot causes the necrosis of the most remote sections of the foot or foot gangrene – gangrene pedis diabetica that due to the complexity of its pathogenesis, should be treated as a separate clinical syndrome. Leg artery disease can result in severe disability.
Diabetic neuropathy
Various kinds of damage to the peripheral nervous system, and its clinical forms are:
Symmetrical sensorimotor peripheral neuropathy characterised by the earlier damage of sensory nerve, lower – of the motor nerves; the lower limbs are predisposed to these changes, and rarely the upper limbs.

The clinical picture
In the initial period: tingling, burning, less impetuous and burning pain in the feet. The symptoms are at rest, intensifying at night under the influence of heat. Sometimes there may appear thermal paraesthesia and the sensation of cold, despite the fact that the feet are warm. Often the “restless legs” symptom appears, forcing them to constant move and change of position.
Mild neuropathy, in which symptoms intensify. Particularly troublesome is the sensation of burning feet. At the same time there are areas with reduced surface sensation, localised mainly in distal sections of the limbs, resembling due to its scope “gloves” or “socks”.
Severe neuropathy causing all forms of disorders to superficial sensation and vibrations. The sensory disturbance is accompanied by physiological reflexes. There appear areas of pain hypoaesthesia, favouring painless injuries. Later on, paresis and muscular atrophy appear, usually affecting foot extensors, small foot muscles, while in the upper limb they affect muscles innervated by the ulnar nerve. The changes in the muscle are accompanied by neurotrophic changes in osteoarthritis.
Focal neuropathy (mononeuropathy) – this complication involves damage to a single sensory or motor nerve, or to several nerves simultaneously, but then these changes are not symmetric and affect nerves in different areas of the body. It is assumed that its immediate cause is sudden ischemia resulting from closure of a nutrient vessel. The main symptoms of mononeuropathy are very strong radiating pain characteristic of the busy nerve and paresis. Mostly the changes affect: the femoral, sciatic, peroneal, median and ulnar nerve. Despite dramatic progress complete recovery can be seen within a few weeks or months.
Autonomic neuropathy is a group of symptoms affecting the autonomic neurons of either or both of the parasympathetic and sympathetic nervous systems.
The clinical picture consists of various syndromes reflecting dysfunctions of individual organs and systems.
Diabetic foot syndrome is a collective term for changes that occur on feet in patients with long-standing diabetes. Their main reason is diabetic specific damage to foot nerves – diabetic neuropathy. It is accompanied by changes in the joints, ligaments and foot bones as well as vascular changes, with causes that the foot is shortened, widened, the longitudinal arch gets deeper. Pressure places appear on the sole, and the reaction of the skin to them is the creation of calluses and cracks in the skin, which are the starting point for infection and foot ulcers.
Pathological changes and clinical symptoms on the lower limbs and feet:
- Changes in the vasculature: atherosclerosis, hardening of the arterioles, microangiopathy of foot tissues, ischemia of soft tissues and bones, formation of infected or not infected necrosis.
- Changes in the innervation of the foot: the loss or impairment of sensory innervation (decrease or loss of pain sensation of pain, temperature, touch, vibration), motor activity (impairment of muscle tension and foot movements, muscle atrophy), autonomic activity (impaired regulation of blood flow through the foot); trophic disorders in the joints (formation of deformations, impaired sweating).
- Skin changes: pale or grey-blue skin, papery, dry, cracked, non-elastic, hair loss, abnormal growth of nails, calluses, necrosis and ulceration.
- Changes in the muscle: muscle weakness, changes in tension, muscle atrophy, contracture.
- Bone abnormalities: bone loss, necrosis, deformations.
Treatment depends on the degree of foot damage. The diagnosis of diabetes begins with conservative treatment. The aim is to metabolic equalisation of the disease, avoid, and preferably completely give up smoking and alcohol consumption, implement an intensive program of general physical exercise and especially foot exercise and their care.
Nosocomial infections are a major problem in modern medicine, because many times they are mean a failure in the treatment and the emergence of complications. The most common problems associated with infections is the lack of aseptic behaviour in the where a medical procedure is performed, a delay in the diagnosis of infection or improper treatment. For the hospital, it is connected with the fact that all these aspects – prevention, diagnosis and treatment – must be done properly.
More and more hospitals decide to obtain an ISO certificate, which leads to the development of procedures for all phases of patient treatment, the observance of which will reduce the number of infections. Moreover, the awareness of the medical staff of this problem is increasing year by year.
The problem of nosocomial infections is also a challenge for manufacturers of medical devices used in the performance of specific procedures in health care units.
The answer to the security needs of the treatment are Matoset products that combine functionality and economy by intentional combining of dressing material. In other words, the individual Matoset is dedicated to a given medical procedure, and particular elements are arranged in a way forcing to perform activities in a particular sequence in accordance with asepsis principles. The structured arrangement and thoughtful composition translates to security, convenience and time saving.
Interview:
Monika Cerkaska – TZMO Product Manager
Katarzyna Moś – Master in Nursing with a specialisation in epidemiological nursing
M.C. In which situations the use of sterile Matoset sets worked best?
K. M. In our daily practice we use Matoset products mainly in treatment rooms, when we have to perform minor medical procedures, such as suture removal or dressing change. Using the sterile sets I am sure that I have all the necessary materials prepared and within a few moments I am able to perform a minor procedure. The ready-for-use sets are indispensable at the patient’s bedside when transporting the patient and performing a procedure in the treatment room is not possible.
M.C. And what about situations when you need to change the dressing at patient’s home?
K. M. Exactly. The health visitor will surely appreciate the comfort of using the sets. It is always certain that all necessary materials are prepared, and each patient has a sense of individual treatment and safety guarantee since the set is designed specifically for him.
M.C. So it much easier to work with the set?
K. M. Yes, it’s easier because they improve the course of a medical procedures, but also thanks to them the work is a lot safer. The arrangement of particular elements determines the actions to be performed. We cannot omit any items e.g. gloves, which are usually placed at the top, and only after their application it is possible to use other sterile components. This minimises the risk of infection, and this is important both for us and for the patient. The documentation process is facilitated by adhesive labels with information about the product, which can be placed in the patient’s records.
M.C. So can we conclude that the sets guarantee the asepsis regardless of the place of performing the procedure?
K. M. Yes, we can. The patient is not always in a place where it is possible to e.g. securely change a dressing. Matoset enables us to do so, and also reduce the time to prepare for the procedure and facilitate the organisation of the work.
M.C. At the end I have to ask – what about the costs?
K. M. The application of complete sets dedicated for a given procedure eliminates the need to open multiple unit packaging, which directly translates into the cost of the procedure. When you open a few packs it increases the possibility of infection of the sterile material. Besides, using the sets – all the content is deliberately used. The rational use of dressing material certainly reduces the cost of its purchase. In addition, medical staff does not have to devote time to complete the dressings for the procedure. In conclusion, I would like to add a few words about the catheter sets and sets for the disinfection of the surgical field, which will surely work well in emergency rooms, although, of course, not only. In situations where time counts, we are not always able to fully observe aseptic rules, the lack of which – as you know – can lead to complications and the cause of prolonged hospitalisation. A patient who is in a life-threatening situation requires undertaking multiple procedures at the same time. The risk of infection while saving lives is greater than during the planned procedures. Therefore, the use of Matoset in the form of ready-for-use sets, such as the catheter set helps to observe the asepsis. A set that contains all the necessary components including an adequate size catheter, allows for the reduction of unnecessary actions to a minimum. The same is true also in the case of the set for disinfecting surgical field, which is justified and fully used up when performing medical procedures in life-threatening conditions. During a resuscitation it is often necessary to apply an endovascular electrode or perform a subclavian vein puncture. Having the complete disinfection set we can take care of the proper preparation of the patient for such procedures in a short time. It is important to save a patient without putting him at any additional risk that after a successful resuscitation may lead to an unwanted contamination. We save the patient and instead “give” him an infection and extended hospital stay. The state of emergency passes, and the patient will require treatment for complications resulting from non-compliance with the basic aseptic principles, the observance of which is certainly facilitated by the Matoset.
M.C. Thank you very much for your time.
‘Wound’ definition
A wound is damage to the skin and sometimes to deeper underlying tissue and even organs as a result of mechanical, thermal or chemical injury. The wounds caused by mechanical injury include: abrasions, cuts, cracks, stab wounds, bite and surgical wounds. The wounds caused by thermal or chemical injury include: all kinds of thermal, chemical, electrical or radiation burns. There are certain types of wounds – chronic (non-healing) wounds, which are caused by other processes – disease processes. Chronic wounds include: pressure ulcers (trophic ulcers), venous ulcers, neuropathic ulcers and ulcers caused by infections and as a result of radiotherapy or neoplastic processes.
Types of wound healing
1. Slowly healing wounds – healing by granulation
- significant loss of tissue
- the wound cannot be closed by using physical methods
- long healing time
- the treatment is based on the processes of tissue reconstruction – the defect fills in with granulation tissue, on which epidermis appears and forms a scar
2. Acute wounds – temporary healing by first intention
- surgical or fresh traumatic wounds
- minimum loss of tissue
- edges are joined by seams or using a plaster
Healing phases
There is no one universal dressing that can be used in each case.
Dressings have different functions: cleansing, absorbent and protective, they often complement each other and none of them alone can meet all the needs of the wound passing through the healing stages:
- inflammation phase (exudate)
- granulation and epithelisation phase (growth)
- maturation phase (reconstruction)
Inflammation phase (exudate)
This phase is the body’s response to an injury. Due to circulatory disorders, enlargement and increased permeability of capillaries oedema occurs, accompanied by exudate.
Functions of the dressing in the inflammation phase:
- stemming the bleeding
- facilitating natural debridement
- absorbing excess exudate
- preventing re-infection
Granulation and epithelising phase (growth)
Granulation – the change from the inflammatory phase into the proliferative phase, which is controlled by macrophages and other cells. Macrophages stimulate fibroblast growth.
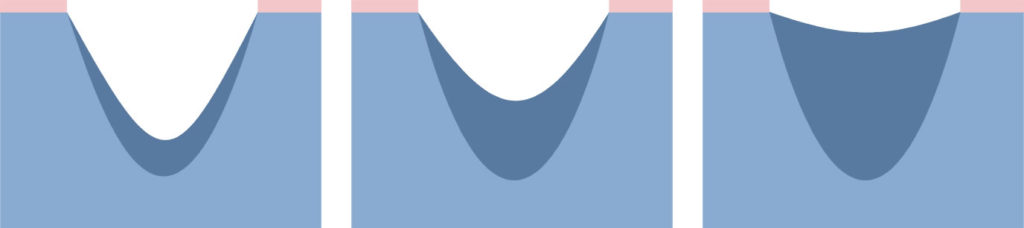
Fibroblasts fill the space that is left after the lost tissue with granulation tissue.
Narrowing of the wound – many fibroblasts is transformed into myofibroblasts. The network of connected myofibroblasts pulls the edges of the wound together (0.6-0.7 mm/day).
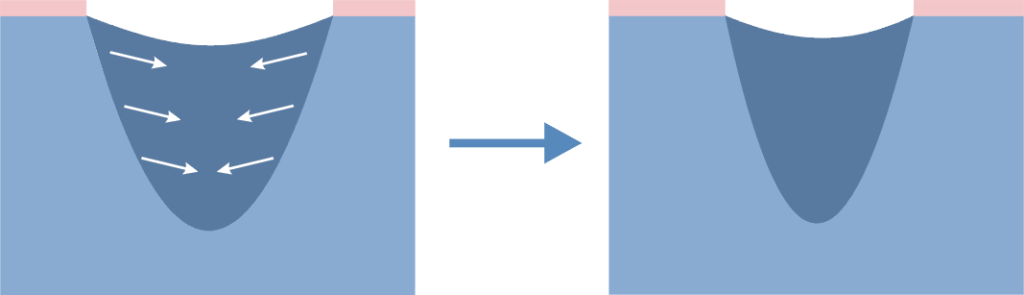
Narrowing of the wound makes the scar smaller than the original wound.
Epithelisation – new epidermis, which is needed for the complete closure of the wound. Epidermal cells migrating from the edges of the wound cover the granulation tissue and create new skin.
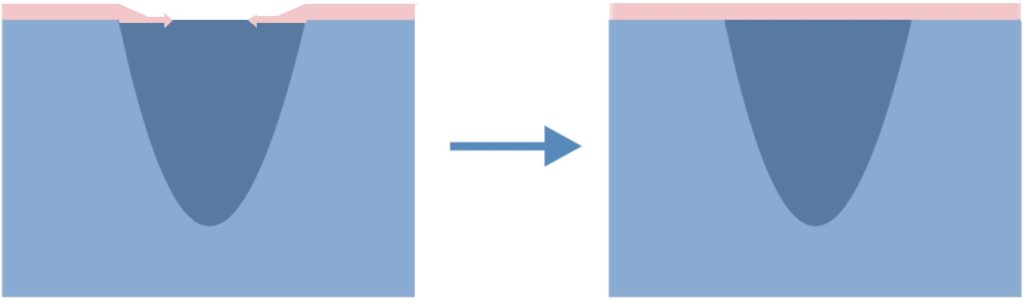
Functions of the dressing in the growth phase:
Granulation
- maintaining moist environment
- absorbing excess exudate
- protecting against mechanical injury
- preventing re-infection
Epithelisation
- maintain a moist environment
- protecting delicate epidermis during dressing changes
Maturation phase
Maturation – slow reorganisation of microscopic structure of scar tissue; the remodelling results in improving the strength of the scar, its reduction and smoothing.
This stage can last for months or even years.
In the treatment of abnormal scarring are the following items are used:
- topical silicone dressings
- compression bandages or special compression garments
- surgery, corticosteroid therapy, laser and cryosurgery
Functions of the dressing in the maturation phase:
- smoothing the scar
- whitening the scar
- reducing the scar
What is wound exudate?
Wound exudate is a particular fluid called in the past “nature balm” appears in the first stage of wound healing, immediately after an injury.
The exudate contains a variety of ingredients including nutrients for actively metabolising cells:
- very few red blood cells
- up to 6 times more white blood cells than in the blood
- less glucose, but the same amount of minerals as the blood
- proteins – among which there are enzymes important for the wound healing processes; the released enzymes cleanse the wound and remove damaged tissues
In a normally healing wound the amount of exudate decreases with time. In a wound, in which the healing process is disturbed, the amount of exudate is not reduced in time and its management can be a big challenge for dressings.
NOTE: to maintain the best possible conditions for wound healing the optimal amount of wound exudate is needed, namely a so-called moist wound healing environment.
Too much exudate and its absence can slow down the healing process. Therefore, it is important to choose an appropriate dressing to the amount of wound exudate. In wounds dry without exudate the dressing should moisten, and in wounds with too much exudate preferably the dressing should absorb its excess.
NOTE: The change in colour, odour and exudate density may indicate a change in the wound or the appearance of inflammation / infection – it is a signal that the wound should be examined and assessed by a specialist.
Dressing type vs. indication for its use in wounds with various exudate amount
| Dressing type | Level of exudate | ||||
| none | low | medium | high | medium/high | |
| challenge for the dressing | hydrate the wound | maintain a moist environment | absorb the excess of exudate | absorb the excess of exudate | drainage of excess exudate to the secondary dressing |
| hydrogel | √ | √ | |||
| polyurethane film | √ | ||||
| hydrocolloid | √ | √ | |||
| polyurethane foam | √ | √ | |||
| alginate | √ | √ | |||
| resorbable | √ | ||||
Wound treatment models
The traditional wound healing model
Through the centuries chronic wounds were treated using a variety of materials that were to dry the wound.
The traditional wound treatment system based on the use of absorbent dressings made of gauze which:
- ensured the absorption of excess exudate
BUT
- failed to protect the wound against drying out and cooling down, which slowed down the rate of healing
- did not constitute adequate protection against external factors, which could lead to frequent wound infections
- adhered to the wound, which damaged the new tissue and caused pain to the patient during dressing changes
- with limited absorptive capacity compelled to frequent dressing change
Dry wound healing is still the most desirable but for acute wounds healing by first intention.
The modern wound healing model
Since the publication of research by George Winter, it became clear that wounds heal much more quickly if the healing process is carried out in humid conditions in which the optimal amount of exudate is maintained on the surface of the wound. In view of the conditions under which the treatment process takes place, the concept was called A MOIST WOUND HEALING.
According to this concept, the treatment deals with closing the wound with a special dressing which:
- maintains the required level of moisture on the wound surface to create an optimal healing environment
- initiates autolytic cleansing, which leads to faster debridement and to start the healing process
- thermally isolates the wound which keeps the temperature at a constant level and accelerates the healing process
- provides long-term absorption of excess exudate, reducing the number of dressing changes
- does not adhere to the wound thanks to which dressing change is safe for young tissues and painless for the patient
- is water-resistant and protects the wound against external environment, which minimises the risk of infection
Features of a perfect dressing
Moist wound healing is most appropriate for hard-to-heal wounds but it can be also used for the treatment of usual cuts, abrasions or scratches.
Hanna Szymkiewicz
European Centre for Long-Term Care
A wound is a skin break, which may extend to deeper tissues and organs. The cause of the wound can be internal and external factors associated with physiological disturbances. The breadth and depth of the wound depends on the causative agent, its strength and areas it affected.
Division of wounds due to the causative agent:
>> exogenous factors:
- mechanical (cut, stab, mashed, gunshot wounds)
- thermal (burns, frostbites)
- chemical (chemical burns)
- electrical (burns)
>> endogenous factors
- ulcers (leg ulcers, pressure sores, diabetic foot) – e.g. impaired circulation
Division of wounds due to the healing time:
- sharp – less than 8 weeks
- chronic – more than 8 weeks
Division of wounds due to the way healing:
- acute wounds – cuts, surgical wounds with even edges and in which there is no substantial loss of tissue. Such wounds are closed with sutures, staples or a dressing, and the wound is healed by first intention and lasts about 6-7 days. It is the most preferred way of healing, and is referred to as primary healing.
- chronic wound – wounds where there is a significant loss of tissue and / or infection. In this case, it is not possible to bring the wound edges together. This type of wound healing by granulation (secondary intention) – the inflammatory phase is followed by proliferative phase, in which the tissue loss is filled with granulation tissue. This process is called secondary healing.
Secondary healing
Secondary wound healing concerns chronic wounds – including bedsores, ulcers, and complicated wounds caused by exogenous factors, such as complex surgical wounds. There are three phases in this healing:
- inflammatory phase (purification)
- proliferation (granulation)
- maturation
The inflammatory phase is characterised by an inflammatory reaction and pain. The body is trying to destroy the bacteria that get into the wound after the discontinuation of the skin. Exudate appears. The dead tissues are excreted out or absorbed by the organism. The wound gets covered with blood clot, which protects it from germs.
In the proliferation phase the exudate is reduced, vessels get narrower, and this is followed by granulation – filling the tissue loss and epithelialisation – the wound is covered with new epidermis.
In the maturation phase the rebuilding process of the newly healed wound takes place to get the strength similar to the intact skin.
The process of healing and its duration depends on many different factors: the general condition of the patient: the age, nutritional status and co-existing diseases; the type of the injury, its location, its closure way, its cleanliness and the time that has passes since the injury to its dressing.